How To Read A Contraction Monitor: Your Essential Guide To Decoding Labor Patterns
How do you read a contraction monitor? This question often arises during the final weeks of pregnancy, bringing a mix of curiosity and anxiety. For many expectant parents, the beeping machine and scrolling paper in a hospital room seem like a complex medical device only professionals can decipher. However, understanding the basic principles of a contraction monitor—officially called a tocodynamometer—is an empowering skill. Whether you're using a home fetal monitor for peace of mind or preparing for a hospital birth, learning to interpret the signals can transform uncertainty into confidence. This guide will walk you through everything you need to know, from the physical device to the patterns that signal your baby's arrival, ensuring you're an active, informed participant in your labor journey.
Understanding how to read a contraction monitor is not about replacing your healthcare provider's expertise but about enhancing your own awareness. It helps you distinguish between practice runs (Braxton Hicks) and the real thing, recognize when it's time to head to the hospital, and communicate more effectively with your birth team. With the rise of remote monitoring and home use, this knowledge is more relevant than ever. So, let's demystify the technology, break down the graphs and numbers, and turn you into a savvy interpreter of your body's most powerful signals.
What Exactly Is a Contraction Monitor?
A contraction monitor is a medical device designed to detect and record uterine activity. Its primary function is to measure the frequency, duration, and intensity of contractions during pregnancy and labor. There are two main types: external and internal. The external monitor, which is most common, uses pressure-sensitive transducers placed on the abdomen. The internal monitor, or intrauterine pressure catheter (IUPC), is a thin tube inserted into the uterus past the cervix, providing more precise measurements but used only in specific clinical situations, typically after the water has broken and in active labor.
The Components of an External Tocodynamometer
An external contraction monitor has two key components: the tocotransducer (for contractions) and the fetal heart rate transducer. The tocotransducer is a flexible belt with a pressure-sensitive button that detects the tightening of the abdominal wall. When a contraction occurs, it pushes against the uterus and the abdominal wall, which the sensor picks up as a rise in pressure. The fetal heart rate transducer uses ultrasound to listen to the baby's heartbeat. Both sensors are connected to a monitor unit that displays the data, traditionally on scrolling graph paper but increasingly on digital screens.
How the Sensors Work: Picking Up the "Tightening"
It's a common misconception that the monitor directly senses the uterine muscle contracting. Instead, the external tocotransductor detects the external manifestation of that contraction: the increased tension and hardness of the abdominal wall. This is why proper placement and snug (but not tight) fitting of the belt are crucial. If the sensor shifts or isn't positioned correctly over the fundus (the top of the uterus), it may miss contractions or give a weak signal. This is also why Braxton Hicks contractions, which are often irregular and localized, might not always be detected as clearly on an external monitor as strong, coordinated labor contractions.
Decoding the Display: What You're Actually Looking At
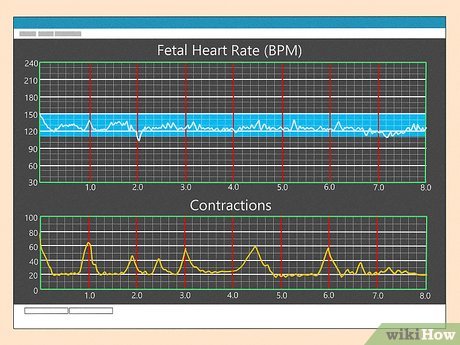
Whether you're looking at a traditional paper strip or a modern digital screen, the information is presented in a consistent format. The display typically shows two graphs scrolling side-by-side or one above the other. The top tracing is almost always the fetal heart rate (FHR), and the bottom tracing is the uterine activity (contractions). Time is marked along the horizontal axis (usually in minutes), and the vertical axis represents either pressure (for contractions) or beats per minute (for the fetal heart rate).
Understanding the Graph Paper: The Classic View
On paper, each small box represents a specific increment of time and pressure. For contractions, the vertical scale is calibrated in Montevideo Units (MVUs) for internal monitors, but for external monitors, it's often just "relative intensity." The height of the contraction peak on the graph does not directly correlate to pain level for the mother; it correlates with the pressure exerted on the abdominal wall. A strong contraction will create a tall, sharp peak on the paper. The baseline (the flat line between contractions) should be at or near zero. A raised baseline can indicate a constant, low-level uterine tension, which is something a provider would monitor.
Digital Readouts: Frequency, Duration, and Intensity
Modern digital monitors provide numerical summaries. You'll see values for:
- Frequency: How often contractions occur, measured in minutes from the start of one contraction to the start of the next (e.g., every 5 minutes).
- Duration: How long each contraction lasts, measured in seconds from the beginning of the rise to the return to baseline (e.g., 60 seconds).
- Intensity/Peak: This is trickier with an external monitor. It's often given as a relative number (e.g., 30-80 mmHg on the pressure scale) or described as "mild," "moderate," or "strong." True quantitative intensity (in Montevideo Units) requires an internal catheter.
The Difference Between Contractions and Peaks: A Critical Distinction
A single "peak" on the graph is one contraction. The monitor doesn't count the number of peaks per minute; it counts the *number of contraction beginnings per 10 minutes. This is why the 5-1-1 rule (contractions 5 minutes apart, lasting 1 minute, for 1 hour) is a guideline for timing from the start of one contraction to the start of the next. A common mistake is to count the peaks themselves within a minute, which would be inaccurate. The space between the peaks is what determines frequency.
Interpreting Contraction Patterns: The Key to Progress
Reading a monitor is about recognizing patterns over time, not just isolated numbers. Labor is a progressive process, and contraction patterns reflect that change. Early labor typically features irregular, longer-interval contractions that may not increase in intensity significantly. As labor progresses into the active phase, contractions become more regular, longer, stronger, and closer together.
The 5-1-1 Rule and Other Clinical Guidelines
The 5-1-1 rule is a classic, practical guideline for when to go to the hospital or call your midwife: contractions that are 5 minutes apart, lasting for 1 minute, and have been occurring consistently for 1 hour. However, this is a general rule for first-time mothers. For those who have had children before, labor often progresses more quickly, so the 4-1-1 or even 3-1-1 rule is often advised. Other clinical parameters focus on the Montevideo Unit (MVU) sum over 10 minutes. For active labor to progress optimally, an internal monitor typically aims for a sum of 200-250 MVUs over a 10-minute window. With an external monitor, you can't calculate MVUs, so you rely on the visual pattern and the 5-1-1 guideline.
Recognizing True Labor vs. Braxton Hicks
This is the most common point of confusion. Braxton Hicks contractions are "practice" contractions. They are usually:
- Irregular and do not get closer together.
- Often felt in the front of the abdomen only.
- May stop with a change in position, hydration, or activity.
- Do not increase in duration or intensity over time.
- Typically last less than 60 seconds and are mild to moderate.
True labor contractions follow a pattern:
- They become progressively more regular.
- They get closer together, longer, and stronger over time.
- They often start in the back and wrap around to the front.
- They do not go away with movement or hydration.
- They are usually accompanied by other signs like the loss of the mucus plug, water breaking, or bloody show.
On a monitor, Braxton Hicks might appear as occasional, isolated peaks with long, flat baselines in between. True labor will show a series of peaks that gradually become taller, closer, and with shorter resting periods between them.
Hyperstimulation and Other Concerning Patterns
A pattern healthcare providers watch for is uterine tachysystole, or hyperstimulation. This is defined as having more than 5 contractions in a 10-minute window, averaged over 30 minutes. This can reduce blood flow to the baby between contractions and is a reason for intervention. On the monitor, it looks like a continuous series of peaks with very little flat baseline in between. Other concerning patterns include contractions that are too long (lasting over 90-120 seconds) or a baseline that is "toney" (elevated and not returning to zero), which can indicate a hypertonic uterus. As a patient, if you're told your contractions are too close or too long, it means the care team is ensuring your baby has adequate recovery time.
Practical Guide: Reading Your Monitor at Home
Many expecting parents rent or purchase home fetal dopplers and contraction monitors for reassurance. While these devices are less sensitive than hospital-grade equipment, they can still be useful for tracking patterns. A crucial disclaimer: Home monitors are for informational and comfort purposes only and are not a substitute for professional medical assessment.
Setting Up and Positioning Sensors Correctly
Placement is everything. The contraction sensor (often a separate, smaller doppler-like device) should be placed on the upper abdomen, just below the rib cage, over the fundus (the top, hard part of the uterus). You may need to move it slightly to find the best spot where the signal is strongest. It should be held in place with an elastic belt or your hand. Ensure your bladder is empty for better contact. A full bladder can create false readings and discomfort. Sit or lie in a comfortable, semi-reclined position.
Timing and Recording Contractions Manually
Even with a monitor, manual timing is a vital backup skill. When you feel a tightening:
- Start a timer (use a contraction app or a simple stopwatch).
- Note the time the contraction begins.
- Note the time the contraction ends (when the tightness completely releases).
- Calculate the duration (end time - start time).
- The time from the start of this contraction to the start of the next is the frequency.
Keep a log. A simple notebook or app that records start time, duration, and intensity (on a 1-10 scale) is invaluable for your provider. Compare your manual log to the monitor's graph to learn what different intensities look like on the screen.
Common Mistakes and How to Avoid Them
- Mistake: Relying solely on the monitor's beep or alarm. Solution: Always correlate the machine's output with what you feel. If the monitor shows a contraction but you felt nothing, it could be a false reading or a very mild Braxton Hicks.
- Mistake: Misinterpreting maternal movement as a contraction. Shifting position, coughing, or the baby's big movements can create a spike on the graph. Solution: Note your activity. If the spike coincides with movement, it's likely not a true contraction.
- Mistake: Poor sensor placement. Solution: Take time to find the "sweet spot." A weak, wavy line often means the sensor needs adjustment.
- Mistake: Panicking over a single reading. Solution: Look for patterns over 30-60 minutes. One strong contraction doesn't mean active labor; a consistent, progressive pattern does.
When to Head to the Hospital: Actionable Thresholds
This is the million-dollar question. The monitor's data helps answer it, but it's only one piece of the puzzle.
The 5-1-1 Rule in Detail (and Its Exceptions)
For a first-time mother (nullipara), the traditional 5-1-1 rule is a safe guideline: contractions 5 minutes apart, lasting 1 minute, for 1 hour. However, if your water breaks at any time, you should go in immediately, regardless of contraction pattern, due to infection risk. For multiparas (those who have given birth before), labor is often faster. Many providers recommend going in at 4-1-1 or even when contractions are 3 minutes apart. Always confirm your specific plan with your provider during your third trimester, as their advice may vary based on your pregnancy history and risk factors.
Other Red Flags That Mean "Go Now"
Contraction pattern is just one signal. Go to the hospital immediately if you experience:
- Your water breaks (a gush or steady trickle of fluid).
- Heavy vaginal bleeding (soaking a pad).
- Decreased fetal movement (fewer than 10 movements in 2 hours, or a significant decrease from your baby's normal pattern).
- Severe, constant pain that doesn't ebb between contractions.
- Fever, chills, or dizziness.
- If you feel something is "not right." Trust your instincts.
What to Tell the Medical Team
When you arrive, communicate clearly:
- "My contractions are [X] minutes apart, lasting about [Y] minutes, and have been this way for [Z] hours."
- "My water broke [how long ago]."
- "I've been timing them manually and/or using a monitor."
- Report any other symptoms (bleeding, fluid, decreased movement).
This concise summary gives them the essential data to prioritize your care.
Advanced Insights: What Your Healthcare Provider Sees
In a hospital setting, the contraction monitor is part of a larger picture. Providers are trained to interpret subtle nuances that go beyond simple timing.
Montevideo Units and Pressure Coupling
When an internal pressure catheter (IUPC) is used, it provides a direct measurement of intrauterine pressure in mmHg. The Montevideo Unit is calculated by summing the peak pressure (above baseline) of each contraction in a 10-minute window. For effective labor progress, the goal is typically >200 MVUs. This quantitative measure helps determine if contractions are adequately strong to dilate the cervix, especially if labor is stalling. It's a much more precise tool than the external monitor's relative intensity scale.
Internal vs. External Monitoring: Accuracy and Use Cases
| Feature | External Tocodynamometer | Internal IUPC |
|---|---|---|
| Measurement | Detects abdominal wall tension | Measures intrauterine pressure directly |
| Accuracy | Good for timing/frequency; less precise for true intensity | Gold standard for quantitative intensity (MVUs) |
| Placement | Belt on abdomen | Catheter through cervix into uterus |
| When Used | Routine labor, early labor, continuous monitoring | Active labor, stalled labor, high-risk cases, after membranes ruptured |
| Mobility | Allows some movement (with wireless) | Confined to bed |
| Discomfort | Minimal | Can be uncomfortable during insertion |
The external monitor is excellent for tracking patterns and frequency, which is 90% of what a laboring person needs to know for the 5-1-1 rule. The internal monitor is a specialized tool for clinical decision-making about augmentation (e.g., Pitocin) or diagnosing true labor arrest.
Conclusion: Empowering Yourself with Knowledge
So, how do you read a contraction monitor? You start by understanding it's a tool that translates your body's powerful work into a visual graph. You learn to identify the peaks (contractions) and the valleys (rest periods). You track the pattern—are they getting closer, longer, and stronger? You correlate the machine's beeps and lines with the sensations in your body. You use tools like the 5-1-1 rule as a general guide, but you also listen to your unique experience and your healthcare provider's personalized advice.
Ultimately, the contraction monitor is a window into the rhythm of labor. Becoming literate in its language doesn't make you a technician; it makes you a more aware and confident participant in one of life's most profound events. It bridges the gap between the internal, often overwhelming experience of labor and the external, objective data that helps everyone on your birth team support you. Armed with this knowledge, you can focus less on deciphering the machine and more on the incredible work your body is doing, trusting that you and your team will recognize the right moment when your baby's journey is ready to begin. Remember, the most important reading is always the one your body and your instincts are telling you.