Why Is My Carotid Artery Visible? Understanding The Causes And When To Worry
Have you ever caught your reflection and noticed a distinct, rhythmic pulse prominently displayed on one side of your neck? That visible carotid artery can be a startling sight, prompting a flurry of questions. Is it normal? Does it mean I have a serious health problem? Is my heart working too hard? The sudden awareness of this vital blood vessel, usually hidden beneath skin and tissue, can trigger understandable concern. This comprehensive guide will delve deep into the anatomy, the common and uncommon reasons for its visibility, how to distinguish between benign and warning signs, and exactly what steps you should take next. Understanding what you're seeing is the first and most crucial step toward peace of mind and proactive health management.
The carotid arteries are two major blood vessels—one on each side of the neck—responsible for delivering oxygen-rich blood from your heart directly to your brain. Their primary function is non-negotiable for consciousness and cognitive function. Under normal circumstances, these arteries are palpable but not typically conspicuous. When they become visibly pronounced, it’s a sign that something has changed in the dynamic between the artery's internal pressure, the surrounding tissue's thickness, or the force of the blood flow itself. This article will serve as your definitive resource, transforming that moment of worry into a clear, actionable understanding of your vascular health.
The Anatomy of Awareness: Your Carotid Artery Up Close
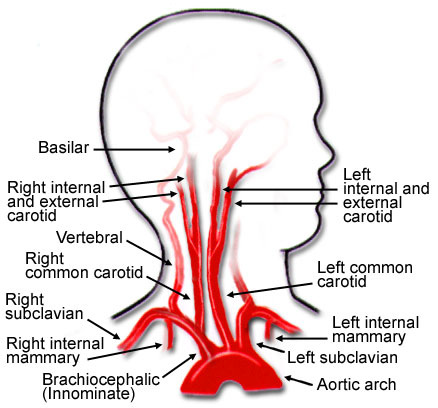
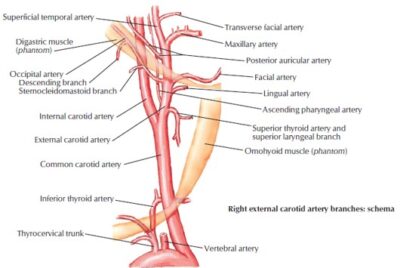
To understand why it might become visible, we must first appreciate what the carotid artery is and its critical location. The common carotid artery branches from the aorta (on the left) or the brachiocephalic trunk (on the right) and travels up the neck. At the level of the thyroid cartilage (the Adam's apple), it bifurcates into the internal carotid artery (which dives deep into the skull to supply the brain) and the external carotid artery (which supplies the face and scalp). The segment most commonly seen pulsating is the common carotid artery just before this bifurcation, lying superficial to the sternocleidomastoid muscle.
Its visibility is a function of three primary physical factors: the force of the blood pressure wave within the vessel (pulse pressure), the thickness of the overlying subcutaneous tissue (fat and skin), and the tension or position of the surrounding muscles. A strong pulse pushing against thin skin will be more obvious than the same pulse beneath a layer of adipose tissue. Furthermore, certain neck postures, like hyperextending the head, can tighten the skin and make the artery's path more apparent. This basic physics principle is the cornerstone of understanding most benign cases of a visible carotid artery.
Normal Variations vs. Potential Red Flags
It is essential to differentiate between a physiologically visible carotid artery and one that signals pathology. For many individuals with a low body fat percentage—such as athletes, bodybuilders, or naturally slender people—the carotid artery is perpetually visible. This is simply due to minimal subcutaneous padding. The pulsation is regular, synchronized with the heartbeat, and not accompanied by any other symptoms like dizziness, pain, or neurological changes. This is a normal anatomical variant, not a disease.
Conversely, a new or suddenly prominent visibility, especially if unilateral (on one side only), warrants closer attention. A pulsatile neck mass that is new, tender, or associated with a bruit (a whooshing sound heard with a stethoscope) could indicate conditions like a carotid artery aneurysm, a carotid body tumor, or significant carotid artery stenosis (narrowing). In stenosis, the blood flow becomes turbulent and forceful distal to the narrowing, sometimes making the artery above the narrowing visibly throb more intensely. This is a critical distinction: long-standing visibility in a thin person is likely benign; a recent change in a person with average or higher body weight is more concerning.
Common Benign Causes of a Prominent Carotid Pulse
Let’s explore the frequent, non-emergent reasons your carotid artery might be putting on a show. These are often related to transient physiological states or inherent body composition.
1. Low Body Fat and Muscle Definition
This is the most common explanation. Individuals with very low body fat percentages (often below 15% for men and 22% for women) lack the insulating layer of subcutaneous fat that typically obscures superficial vessels. The carotid artery lies in a relatively shallow groove, making it prone to visibility. Bodybuilders pre-competition, long-distance runners, and those with a naturally ectomorphic (slender) build often exhibit this. The pulsation is symmetrical, strong, and completely benign. It’s a testament to your physique, not a flaw in your health.
2. Temporary Increases in Cardiac Output
Your heart pumps harder and faster during exercise, emotional arousal (like anxiety or excitement), or when fighting an illness (fever). This increases stroke volume and heart rate, leading to a more forceful pulse wave throughout the arterial system. You might notice your carotid (and other arteries, like in your wrist) pulsing more vigorously after a strenuous workout or during a panic attack. This is temporary and resolves as your heart rate and blood pressure return to baseline. Dehydration can also concentrate blood volume and slightly elevate heart rate, making pulses more apparent.
3. Hypertension (High Blood Pressure)
Consistently elevated blood pressure increases the force against the arterial walls with every heartbeat. Over time, this can make the pulse pressure (the difference between systolic and diastolic pressure) more noticeable. If you have undiagnosed or uncontrolled hypertension, you might observe a firmer, more robust pulsation in your neck. This is a significant reason to have your blood pressure checked regularly. Hypertension is a major risk factor for atherosclerosis and carotid artery disease, so this visibility can be an early, visual cue to address a silent condition.
4. Aging and Loss of Skin Elasticity
As we age, our skin loses collagen and elastin, becoming thinner and less taut. Simultaneously, the layer of subcutaneous fat may redistribute or decrease. This combination can make underlying structures, including arteries, more visible. The loss of youthful plumpness in the neck area is a common cosmetic change, and the resulting visibility of tendons, veins, and arteries is part of that process. While aging itself is inevitable, the associated vascular changes should still be monitored for signs of disease.
Medical Conditions That Can Cause a Visible Carotid Artery
When visibility is new, asymmetric, or associated with other symptoms, it’s time to consider underlying medical conditions. These require professional diagnosis.
Carotid Artery Stenosis (Narrowing)
This is the buildup of plaque (fat, cholesterol, calcium) on the inner walls of the carotid artery, a process called atherosclerosis. It’s a serious condition because it can lead to stroke. As the artery narrows, blood flow velocity increases to maintain volume (think of putting your thumb over a garden hose), creating turbulent flow. This turbulence can cause a strong, palpable thrill or a audible bruit (heard with a stethoscope). In some cases, the increased pressure and turbulence proximal to the severe narrowing can make that segment of the artery appear to pulse more forcefully. Risk factors include smoking, diabetes, high cholesterol, hypertension, and age. A visible carotid artery in an older adult with cardiovascular risk factors should never be ignored.
Carotid Artery Aneurysm
An aneurysm is a localized, balloon-like dilation of the artery wall. A carotid artery aneurysm is rare but serious. It presents as a soft, compressible, pulsatile mass at the site of the aneurysm. It may be tender and is almost always unilateral. Aneurysms can be true (involving all three vessel wall layers) or pseudoaneurysms (a leak contained by surrounding tissue). They carry a risk of rupture or embolism (clot breaking off). Any new, distinct, pulsatile lump—not just a visible artery—needs urgent vascular evaluation.
Carotid Body Tumor (Paraganglioma)
Also known as a chemodectoma, this is a rare, usually benign tumor that arises at the carotid bifurcation where the common carotid splits. It grows between the internal and external carotid arteries. Classically, it presents as a painless, slow-growing, firm, mobile mass that is not directly pulsatile but may transmit pulsations from the adjacent arteries (a "pulsatile on top of pulsatile" feel). It is often discovered incidentally. While typically benign, about 5-10% can be malignant or secrete hormones, so evaluation is necessary.
Tortuosity or Kinking of the Carotid Artery
Some people are born with or develop an abnormally twisted or looped carotid artery, a condition called tortuosity. This can make the artery’s path more superficial and visible in certain neck positions. It’s often an incidental finding on imaging (like a carotid ultrasound or CT angiogram) and is usually asymptomatic. However, extreme kinking can, in rare cases, compromise blood flow to the brain, especially with head rotation, leading to dizziness or transient ischemic attacks (TIAs).
How to Perform a Basic Self-Check: What to Look For
While not a substitute for a medical exam, a mindful self-assessment can provide useful information for your doctor.
1. Locate and Observe: Sit in a well-lit room, head in a neutral position. Use a mirror to identify the pulsation. Is it on one side or both? Is it a straight line or does it follow a curved path? Is the pulsation rhythmic and consistent with your heartbeat?
2. Palpate Gently: Place your fingertips (not your thumb, as it has its own pulse) lightly on the site. Feel for the pulse. Is it strong, bounding, or normal? Is there a palpable thrill (a vibrating sensation)? Can you feel a discrete mass separate from the artery's pulsation?
3. Listen with Caution: In a very quiet room, you might hear a soft "whooshing" sound synchronous with your heartbeat. This is normal in very thin people. However, a loud, harsh, or blowing sound (a bruit) heard without a stethoscope, or clearly with one, suggests turbulent flow and needs evaluation.
4. Perform the "Head Turn" Test: Gently turn your head fully to the opposite side of the visible artery. Does the pulsation become more pronounced, less visible, or unchanged? Does this movement cause any dizziness, vision changes, or weakness? A change with rotation can suggest kinking or compression.
5. Monitor for Associated Symptoms: This is the most critical part. Be alert for:
- Neurological: Sudden weakness/numbness (especially one-sided), difficulty speaking, vision loss/blurriness, severe dizziness/loss of balance. (These are stroke symptoms—call emergency services immediately).
- Local: Pain, tenderness, or rapid growth of the area.
- Systemic: Unexplained weight loss, night sweats (can signal rare tumors).
- Cardiac: Palpitations, chest pain, shortness of breath.
Diagnosis: What to Expect at the Doctor's Office
If you decide to seek medical advice—which you should for any new, unilateral, or symptomatic finding—your physician will follow a logical diagnostic pathway.
History and Physical Exam: Your doctor will ask about onset, duration, associated symptoms, and your cardiovascular risk factors (smoking, hypertension, diabetes, family history). They will visually inspect and palpate your neck, listening carefully with a stethoscope for a carotid bruit. They will also perform a full neurological exam.
Carotid Duplex Ultrasound: This is the first-line, non-invasive, and painless diagnostic test. It uses sound waves to create images of the carotid arteries and measures blood flow velocity. It can accurately detect stenosis (narrowing), plaque characteristics, and turbulent flow. It’s like a real-time video of your artery’s health and is completely safe, using no radiation or dye.
Further Imaging: If the ultrasound is inconclusive or shows a complex abnormality, your doctor may order:
- CT Angiography (CTA): Uses contrast dye and X-rays to create a 3D map of your arteries. Excellent for viewing anatomy and plaque.
- Magnetic Resonance Angiography (MRA): Uses magnetic fields and often contrast dye to visualize vessels. Good for soft tissue detail.
- Catheter-based Cerebral Angiography: The gold standard, but invasive. A catheter is threaded from an artery in your groin up to your neck to inject dye and take precise X-rays. Used when other tests are unclear or before surgery.
Treatment and Management Strategies
Treatment is entirely dependent on the underlying diagnosis.
For Benign Visibility (Low Body Fat):No treatment is needed. Reassurance is the key. Maintain a healthy lifestyle, but understand this is your normal anatomy.
For Hypertension: Aggressive management with lifestyle changes (DASH diet, exercise, sodium reduction, stress management) and antihypertensive medications is essential. Controlling blood pressure reduces pulse pressure and long-term arterial damage.
For Carotid Artery Stenosis: Treatment depends on severity.
- Mild to Moderate (50-69% stenosis): Intensive medical management: antiplatelet therapy (e.g., aspirin), statin medications to lower cholesterol, strict blood pressure and diabetes control, smoking cessation, and lifestyle modifications.
- Severe (70-99% stenosis) or Symptomatic (caused a TIA or mini-stroke):Revascularization is typically recommended. This is either:
- Carotid Endarterectomy (CEA): Open surgery to remove the plaque.
- Carotid Artery Stenting (CAS): A less invasive procedure where a stent is placed to prop the artery open via a catheter.
For Aneurysm or Tumor: Surgical resection or endovascular repair (for aneurysms) is almost always indicated. Treatment for carotid body tumors is surgical excision, often requiring careful planning to preserve nearby nerves.
Prevention: Protecting Your Carotid Arteries for Life
Whether you have a visible artery or not, proactive care for your vascular system is non-negotiable for long-term health.
- Know Your Numbers: Regularly monitor and control your blood pressure, cholesterol (LDL), and blood sugar.
- Adopt a Heart-Healthy Diet: Emphasize vegetables, fruits, whole grains, lean proteins, and healthy fats (omega-3s). Minimize processed foods, trans fats, and excess sodium and sugar.
- Exercise Regularly: Aim for at least 150 minutes of moderate aerobic activity (brisk walking, cycling) per week. Exercise improves endothelial function and lowers blood pressure.
- Never Smoke, and Avoid Secondhand Smoke: Smoking is the single most potent accelerator of atherosclerosis.
- Maintain a Healthy Weight: Reduces strain on your cardiovascular system.
- Manage Stress: Chronic stress contributes to inflammation and hypertension. Practice mindfulness, meditation, or yoga.
- Regular Check-ups: See your primary care physician annually for a cardiovascular risk assessment. Discuss any new findings, like a visible carotid pulse, promptly.
Frequently Asked Questions (FAQs)
Q: Is a visible carotid artery always a sign of high blood pressure?
A: No. While hypertension can cause a bounding pulse, the most common cause is simply low body fat. However, it can be a sign of hypertension, which is why checking your blood pressure is a crucial first step.
Q: Can I feel my carotid artery to check my pulse?
A: Use extreme caution. You can gently palpate one side at a time to feel the pulse rate. Never apply pressure to both carotid arteries simultaneously, as this can stimulate baroreceptors and potentially cause dizziness or fainting. Never massage or vigorously rub the area.
Q: My carotid artery is visible and I have a family history of stroke. Should I be worried?
A: Yes, this combination warrants a medical evaluation. A family history of early stroke or heart disease increases your baseline risk. A visible carotid artery in this context should be assessed with a carotid duplex ultrasound to rule out significant stenosis.
Q: Does a visible carotid artery mean I have an aneurysm?
A: Almost certainly not. Aneurysms are rare. A visible carotid artery is usually just the normal vessel seen through thin tissue. An aneurysm would present as a distinct, soft, compressible, and often tender lump that is pulsatile, not just a visible linear pulsation.
Q: Can exercises or neck movements make it worse?
A: Strenuous exercise that spikes your heart rate will temporarily make any pulse more forceful. Certain neck positions (hyperextension) can make it more visible. However, normal exercise and movement do not "damage" a healthy carotid artery. If specific neck rotations cause neurological symptoms (dizziness, vision changes), that is a sign to stop and see a doctor.
Conclusion: Knowledge is Your Greatest Ally
The sudden discovery of a visible carotid artery in your neck is a moment that bridges anatomy and anxiety. For the vast majority, it is a harmless consequence of a lean physique or a temporary spike in cardiac output—a simple matter of physics and personal biology. However, it can also be the body's subtle billboard advertising underlying vascular stress, from uncontrolled hypertension to significant arterial narrowing. The critical path forward is not panic, but purposeful observation and informed action.
Your strategy should be this: first, perform a calm, mindful self-assessment as outlined. Note its characteristics, symmetry, and any associated symptoms. Second, know your cardiovascular risk factors—your blood pressure, cholesterol, smoking status, and family history are your most important data points. Third, and most importantly, share your observation with a healthcare professional. A simple, painless carotid ultrasound can provide definitive answers, ruling out serious conditions or identifying them at a stage where intervention is most effective. Whether the outcome is benign reassurance or a life-saving treatment plan, taking that step transforms uncertainty into control. Your carotid arteries are the lifelines to your brain; honoring their health with awareness and appropriate care is one of the most profound investments you can make in your long-term well-being.