What Does A Dry Socket Look Like? A Visual Guide To This Painful Dental Complication
Have you recently had a tooth extracted, only to find that the pain isn't subsiding—it's actually getting worse a few days later? You might be staring into your mouth with a mirror, wondering, what does a dry socket look like? It’s a frightening question for anyone recovering from a dental procedure. The fear of the unknown, coupled with intense, radiating pain, can be deeply unsettling. This comprehensive guide will walk you through exactly what a dry socket is, provide a detailed visual description, explain why it happens, and most importantly, tell you what to do if you suspect you have one. Understanding the signs can empower you to seek timely treatment and get relief.
Dry socket, medically known as alveolar osteitis, is a common but painful complication that can occur after a tooth extraction. It happens when the blood clot that should form in the empty socket either fails to develop, dissolves prematurely, or is dislodged. This clot is crucial—it protects the underlying bone and nerves and serves as the foundation for new tissue growth. Without it, the bone and nerves are exposed to air, food, and bacteria, leading to significant pain and delayed healing. While only affecting about 2-5% of all extractions, its incidence jumps to a higher percentage with more complex surgical removals, like impacted wisdom teeth.
This article will serve as your complete visual and informational reference. We’ll move from the basic definition to a step-by-step visual breakdown, explore the science behind the symptoms, detail causes and risk factors, and provide clear, actionable advice on treatment and prevention. By the end, you’ll know precisely what to look for, understand the "why" behind the pain, and feel confident in the next steps to take.
Defining the Condition: What Exactly Is a Dry Socket?
Before we dive into visuals, it’s essential to understand the fundamental process a dry socket disrupts. A normal tooth extraction site follows a predictable healing cascade. Immediately after the tooth is removed, bleeding occurs, and your body’s natural response is to form a blood clot within the empty alveolar socket. This clot is not just a plug; it’s a living, bioactive scaffold. It stops bleeding, shields the raw bone and nerve endings from the oral environment, and contains the cells necessary to begin the regeneration of gum tissue and bone.
A dry socket (alveolar osteitis) occurs when this protective clot is lost or never forms properly. The term "dry" refers to the socket’s appearance—it appears empty, dry, and may have a grayish or creamy white exposed bone surface. The loss of the clot exposes the highly sensitive periosteum (the membrane covering the bone) and nerve endings. This exposure is the primary driver of the characteristic severe, throbbing pain. Furthermore, the empty socket becomes a breeding ground for bacteria, leading to inflammation and a foul odor, which compounds the discomfort.
The timeline is a key diagnostic clue. Pain from a normal extraction should gradually lessen each day. With a dry socket, there is often a deceptive period of relief for the first 1-3 days post-extraction. Then, typically between days 3 to 5 after the procedure, pain escalates dramatically. This delayed onset is a classic hallmark that helps differentiate it from normal post-operative pain.
The Visual Breakdown: A Step-by-Step Look at a Dry Socket
So, you’re peering into the mirror with a flashlight. What, exactly, should you be looking for? The visual presentation is distinct from a healthy healing socket. Let’s break it down layer by layer.
The Healthy Healing Socket (For Comparison)
First, know what normal looks like. A healthy socket 2-4 days after extraction will have a dark red or dark brownish blood clot filling the space where the tooth was. It may look gelatinous or firm. The surrounding gum tissue will be slightly swollen and red, but the socket itself is plugged. There is no exposed bone visible to the naked eye. The pain should be manageable with over-the-counter medication and improving steadily.
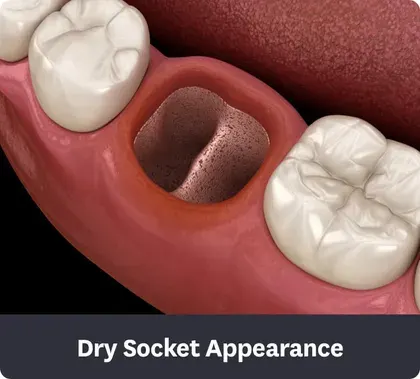
The Dry Socket Appearance: Key Visual Indicators
When you look at a suspected dry socket, you are likely seeing one or more of the following:
- An Empty or Partially Empty Socket: The most obvious sign is the absence of a blood clot. The socket may look like a small, dark hole. In some cases, a small, fragmented clot might be present at the bottom, but the majority of the socket is devoid of the protective plug.
- Exposed Bone: This is the definitive visual feature. Without the clot covering it, you may see a smooth, shiny, bone surface. It often appears creamy white, gray, or yellowish in color. This is the actual jawbone (alveolar bone) that held the tooth. It may look like a tiny, polished pebble at the bottom of the socket.
- Discolored or Necrotic Tissue: The tissue lining the socket walls (the socket epithelium) can become inflamed and die (necrosis) due to lack of blood supply and bacterial invasion. This can appear as a yellowish, tan, or greenish film coating the exposed bone or the socket walls. This is not a healthy granulation tissue (which is pink and fleshy) but a sign of infection and poor healing.
- Foul Odor and Taste: While not a "look," it’s an undeniable sensory clue accompanying the visual. A persistent, unpleasant metallic or foul smell emanating from the socket, and a corresponding bad taste in your mouth that doesn't go away with rinsing, is strongly associated with dry socket. This results from the breakdown of exposed bone and bacterial colonization in the empty space.
Important Note: It can be very difficult to see your own molars and wisdom teeth clearly. If you suspect a problem, the best visual assessment will come from your dentist or oral surgeon. They have the tools (light, mirrors, suction) to get a clear, safe view.
The Symphony of Symptoms: Pain, Odor, and Empty Feeling
The visual cues are just one part of the diagnostic picture. The symptom complex is what truly defines a dry socket and sends patients seeking urgent care.
- Severe, Radiating Pain: This is the cardinal symptom. The pain is not confined to the socket. It is often described as sharp, throbbing, or burning and can radiate to the ear, temple, eye, or neck on the affected side. It is frequently worse at night and can be unrelenting, barely eased by typical post-op pain medications.
- Delayed Onset: As mentioned, pain that disappears for a couple of days only to return with vengeance around day 3-5 is a major red flag.
- Visible Empty Socket: As described above.
- Bad Breath and Taste (Halitosis): The foul odor and persistent bad taste are nearly universal complaints.
- Swollen Lymph Nodes: The lymph nodes under the jaw or in the neck on the affected side may become tender and swollen as your body fights the local inflammation and infection.
- "Feeling" the Bone: Some patients report a strange sensation of being able to "feel" the air or food hitting the exposed bone when they eat or breathe.
The "Why": Causes and Risk Factors Explained
Understanding why a dry socket occurs helps in both diagnosis and prevention. It’s rarely a single cause and usually a convergence of factors that disrupts clot stability.
Primary Mechanical Causes:
- Suction: Using a straw creates negative pressure in the mouth that can physically suck the clot out of the socket. This is the most commonly advised against activity.
- Rinsing and Spitting Vigorously: Forceful rinsing, especially within the first 24 hours, or aggressive spitting can dislodge the fragile clot.
- Trauma from Food: Hard, crunchy, or small, sharp foods (like chips, seeds, popcorn kernels) can get lodged in the socket and displace the clot as you chew.
Biological and Chemical Causes:
- Fibrinolysis: This is the body's own process of breaking down blood clots. In some individuals, an exaggerated fibrinolytic response occurs at the extraction site, causing the clot to dissolve prematurely.
- Bacterial Infection: Certain bacteria present in the mouth can produce enzymes that break down the clot or prevent its formation in the first place.
- Pre-existing Infection: If the tooth was extracted due to an active abscess or infection, the surrounding tissues and environment are already compromised, making clot formation and stability much harder.
Major Risk Factors:
- Complex Extractions: Surgical removal of impacted wisdom teeth, especially lower ones, involves more bone removal and trauma. This significantly increases the risk (up to 30% in some studies).
- Smoking and Tobacco Use: Nicotine constricts blood vessels, impairing blood flow and clot formation. The act of inhaling also creates suction. Smokers are at a 2-4 times higher risk.
- Oral Contraceptives: Women on birth control pills have higher levels of estrogen, which can increase fibrinolytic activity and risk. The risk is highest during the placebo pill week (days 22-28 of the cycle).
- Previous History of Dry Socket: If you’ve had one before, you are at a significantly higher risk of recurrence.
- Poor Oral Hygiene: Inadequate cleaning allows bacterial load to build up.
- Age: Higher incidence is seen in individuals in their 20s and 30s, possibly related to denser bone and more frequent extractions of impacted teeth in this age group.
- Systemic Conditions: Uncontrolled diabetes or other conditions affecting blood flow and healing.
Treatment: What Your Dentist Will Do
If you suspect a dry socket, contact your dentist or oral surgeon immediately. Treatment is not something to delay or attempt at home beyond initial pain management. The goals are to manage pain, promote healing, and clean the socket.
The standard in-office treatment involves:
- Gentle Irrigation: The dentist will thoroughly flush the socket with a sterile saline or antimicrobial solution to remove any debris, food particles, and bacterial biofilm. This is done carefully to avoid further trauma.
- Medicated Dressing: This is the cornerstone of treatment. The dentist will pack the clean socket with a special medicated dressing (often containing eugenol, a clove oil derivative, which has analgesic and antiseptic properties). This dressing:
- Provides immediate pain relief by physically blocking the exposed nerve endings from air and irritants.
- Creates a moist, protected environment that encourages new clot formation.
- Delivers sustained antimicrobial medication directly into the socket.
- Prescription Pain Relief: You will likely be prescribed a stronger pain medication than what you were given post-operatively.
- Antibiotics: These are not always given, as dry socket is not a classic infection but an inflammatory condition. However, if there are signs of spreading infection (fever, increasing swelling), antibiotics will be prescribed.
- Follow-up Care: You’ll need to return to the office every 1-3 days for dressing changes until the socket shows signs of healing (new tissue formation, pain subsiding). Healing typically takes 1-2 weeks with proper care.
At-Home Care During Treatment:
- Rinse Gently: After the first 24 hours, rinse very gently with warm salt water (1/2 tsp salt in 8 oz water) after meals to keep the area clean. Do not swish vigorously; let the water fall out of your mouth.
- Diet: Stick to soft, cool foods on the opposite side of the mouth. Avoid hot liquids, alcohol, and anything that could disturb the socket.
- Oral Hygiene: Brush your teeth carefully, avoiding the immediate area for the first few days. Do not use a toothbrush directly in the socket.
- Avoid Suction: Absolutely no straws, smoking, or vaping.
Prevention: Your Proactive Action Plan
Prevention is always preferable to treatment. If you’re scheduled for an extraction, especially a surgical one, take these steps:
- Quit Smoking: Stop at least 72 hours before and 72 hours after the procedure. This is the single most effective preventive measure for smokers.
- Discuss Medications: Inform your dentist about all medications, especially birth control pills. They may advise scheduling the extraction during the low-estrogen phase of your cycle (days 1-14) to reduce risk.
- Pre- and Post-Op Rinses: Some studies suggest rinsing with an antimicrobial mouthwash (like chlorhexidine) before and after extraction can reduce bacterial load. Your dentist may recommend this.
- Protect the Clot: Follow all post-op instructions meticulously:
- No straws for at least 7 days.
- Avoid spitting forcefully for 24-48 hours; let liquids drip from your mouth.
- Eat only soft foods for the first few days.
- Do not probe the socket with your tongue or any object.
- Consider Sutures: For high-risk extractions, ask your surgeon about using sutures to help stabilize the clot.
- Maintain Excellent Oral Hygiene: Keep your mouth clean, but be gentle around the extraction site.
When to Call the Dentist: A Simple Checklist
Don’t wait in agony. Seek professional help if you experience any of the following after an extraction:
- Pain that increases after the 2nd or 3rd day, rather than decreasing.
- Pain that radiates to your ear, temple, or neck.
- A visible empty socket or exposed bone.
- A persistent foul taste or odor that won’t go away.
- Swelling that gets worse after the third day.
- Fever or general malaise.
Addressing Common Questions
Q: Can I treat a dry socket at home?
A: While saltwater rinses can help keep it clean, professional treatment is required for pain relief and proper healing. The medicated dressing is a specific medical application.
Q: Is a dry socket contagious?
A: No. It is not an infectious disease you can catch from someone. It’s a localized inflammatory condition at your extraction site.
Q: How long does it take to heal?
A: With proper dental treatment, significant pain relief is often felt within 24-48 hours of the first dressing. Complete healing of the socket takes about 1-2 weeks.
Q: Can I eat with a dry socket?
A: Yes, but stick to soft, cool foods on the opposite side of your mouth. Avoid hot, spicy, crunchy, or chewy foods that can irritate the socket or dislodge a new forming clot.
Q: Will I get a dry socket with every extraction?
A: No. The risk is relatively low for simple extractions. Your risk profile depends on the factors listed above (smoking, surgery complexity, etc.).
Conclusion: Knowledge is Your Best Defense
The question "what does a dry socket look like?" is more than a curiosity—it’s a vital piece of self-awareness for anyone undergoing a tooth extraction. The visual hallmarks—an empty socket, exposed creamy-white bone, and yellowish necrotic tissue—combined with the telltale delayed, severe, radiating pain and foul odor, form a clear clinical picture. Remember, this condition is a disruption of the natural, protective healing process.
While the experience is undoubtedly painful, it is highly treatable with prompt professional intervention. The key is recognizing the signs early and not dismissing worsening pain as "normal." Your dentist has effective tools—irrigation, medicated dressings, and pain management—to provide relief and set your healing back on track. More powerfully, you can take proactive, evidence-based steps to prevent it by following post-operative instructions to the letter, avoiding suction, and communicating your risk factors (like smoking) to your surgeon.
Ultimately, your oral health journey doesn’t end when you leave the dental chair. Being an informed, vigilant patient in the days and weeks following a procedure is your greatest asset. If your pain story after an extraction doesn’t follow the expected script of steady improvement, trust your instincts. Look, assess your symptoms, and contact your dental professional without hesitation. Fast action means faster relief and a quicker return to a healthy, comfortable smile.