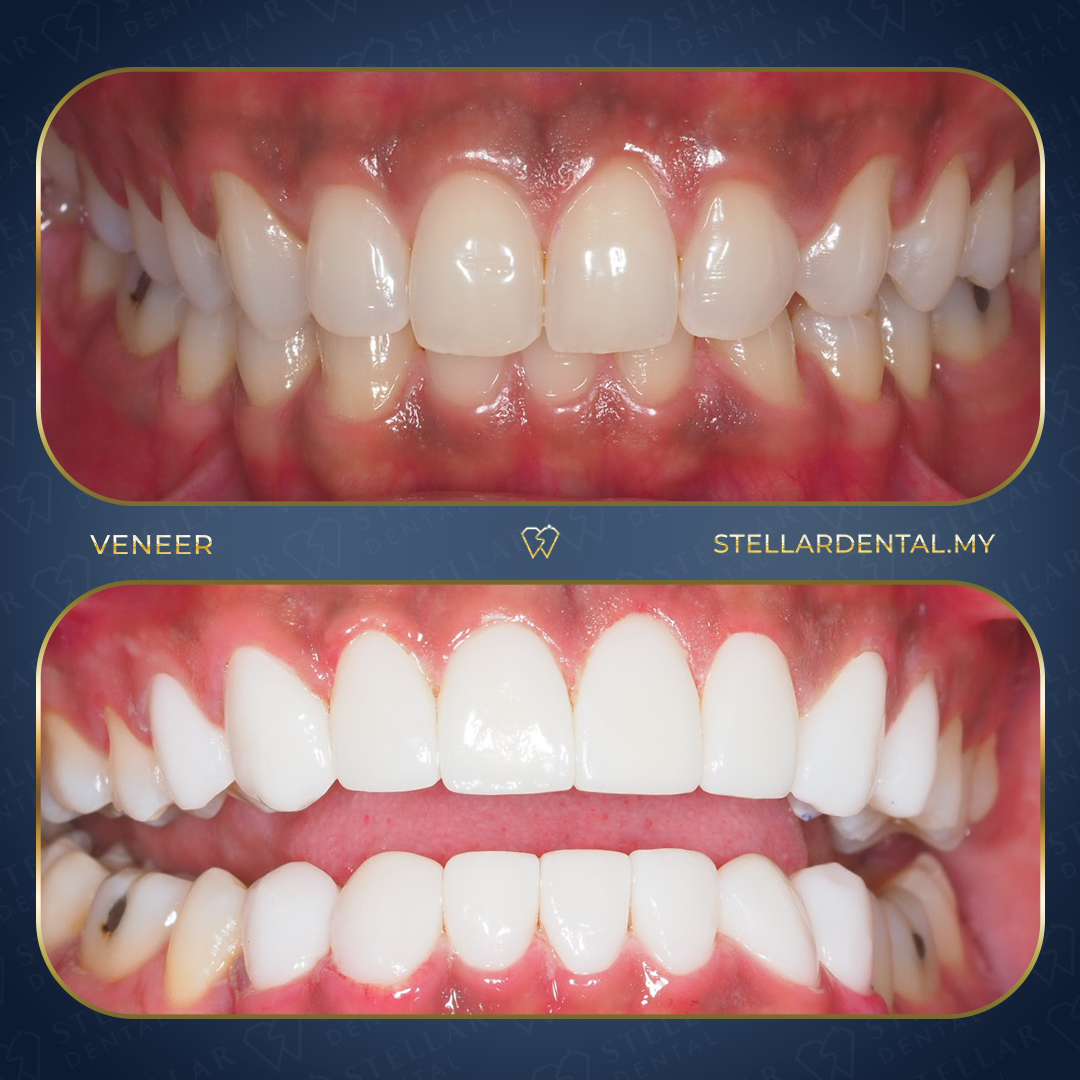
The Shocking Truth About Bad Veneers: Before And After Disasters Exposed
Have you ever scrolled through social media and seen a celebrity’s smile look… off? Maybe the teeth are unnaturally white, oddly shaped, or seem to be sitting strangely in the gums? You’re not just being critical—you might be looking at the classic signs of bad veneers before and after a poorly executed procedure. The dream of a perfect, Hollywood-worthy smile can quickly turn into a dental nightmare when things go wrong. This isn’t just about aesthetics; it’s about oral health, function, and confidence. In this comprehensive guide, we’ll pull back the curtain on cosmetic dentistry failures. We’ll show you exactly what bad veneers look like, the common mistakes that cause them, and, most importantly, how to avoid becoming a victim of a before and after story you never wanted.
The promise of veneers is simple: a custom-made, thin shell of porcelain or composite resin bonded to the front of your teeth to correct discoloration, chips, gaps, or misalignment. When done by a skilled cosmetic dentist with meticulous planning, the results can be life-changing. However, the inverse is also true. A cascade of poor decisions—from inadequate diagnostic work to subpar lab work and careless bonding—can lead to results that are not only aesthetically displeasing but also functionally harmful. Understanding these failures is the first step toward ensuring your own smile transformation is a success story, not a cautionary tale.
The Anatomy of a Veneer Disaster: Common Failure Modes
1. The "Chiclet" or Artificial Smile: Poor Color and Opacity Matching
One of the most frequent and glaring signs of bad veneers before and after photos is a smile that looks uniformly fake. This often stems from a catastrophic failure in color selection and characterization.
What it looks like: The veneers are a single, flat shade of bright white—often the brightest shade on the dental chart—with no variation, translucency, or depth. They look more like pieces of plastic or acrylic than natural teeth. In before and after comparisons, the "after" smile lacks the subtle hints of blue, gray, or yellow that give real teeth their lifelike quality. The opacity is wrong; sometimes they are too opaque and chalky, other times too translucent, revealing a dark or discolored underlying tooth underneath.
Why it happens: This is a lab and planning failure. The dentist may have selected a shade based solely on a standardized chart without considering the patient’s skin tone, facial features, and the natural gradient of color in a healthy dentition. A high-quality cosmetic lab will hand-characterize each veneer, layering different shades and translucencies to mimic the natural tooth structure. A cheap, rushed lab will simply press a uniform block of porcelain. The dentist’s responsibility is to communicate the desired aesthetic and approve the lab’s mock-up (a wax or resin trial set) before the final veneers are fabricated.
The Fix: Prevention is everything. A proper smile design consultation using digital mock-up software is non-negotiable. You should see exactly what your new smile will look like before any tooth preparation. If the proposed shade looks flat, speak up. Ask to see samples with different levels of characterization. For existing bad veneers, correction often requires complete replacement. The old veneers must be removed, and the teeth may need additional preparation to correct the underlying issues before new, properly characterized veneers are bonded.
2. The "Wrong Size" Problem: Unnatural Shape and Proportions
Natural teeth have specific, harmonious proportions. The central incisors are typically the widest, with the lateral incisors and canines tapering gracefully. When this anatomy is ignored, the result is a smile that draws attention for all the wrong reasons.
What it looks like: Veneers that are all the same width, creating a "buck-toothed" or overly broad appearance. They might be too long, causing the teeth to appear crowded or to overlap the lower lip unnaturally when smiling. Conversely, they might be too short, making the smile look aged and gummy. In severe cases, the veneers may have a rectangular, boxy shape instead of the gentle curvature of natural incisal edges.
Why it happens: This is a fundamental flaw in the smile design phase. The dentist or lab technician failed to use established aesthetic principles like the "Golden Proportion" or the "Red Centaur" aesthetic guidelines. They may have used a one-size-fits-all template or simply didn't account for the patient’s unique facial features, lip dynamics, and gum contours. A common mistake is making laterals (the teeth next to the centrals) too wide, which disrupts the smile's rhythm.
The Fix: A meticulous diagnostic process involving digital smile design (DSD) and a physical mock-up (try-in) is critical. The mock-up, placed on your teeth with temporary cement, allows you to see and feel the proposed shape and size in your own mouth, in motion, while talking and smiling. If the shape is wrong during this stage, it must be adjusted before the permanent veneers are made. Correcting existing bad veneers with poor shape usually means a full remake, often requiring careful re-preparation to achieve the correct new tooth form.
3. The "Black Line" Blues: Visible Margins and Over- or Under-Contouring
Perhaps one of the most tell-tale and easily avoidable signs of bad veneers is a dark line at the gumline. This is a clear indicator of poor marginal adaptation and execution.
What it looks like: A thin, dark gray or black line appears where the veneer meets the gum. This can be because the veneer was placed too far subgingivally (under the gum), irritating the tissue and creating a shelf for plaque. Alternatively, the margin might be over-contoured, meaning the veneer bulges out at the edge, creating a ledge that traps food and bacteria. The opposite, under-contouring, can create a visible gap or "open margin."
Why it happens: This is a pure craftsmanship failure, usually at the dentist's hand during tooth preparation or bonding. The preparation must follow a precise, smooth, and consistent margin at or slightly above the gumline. If the dentist over-prepares or creates an uneven edge, the lab cannot fabricate a perfect-fitting veneer. During bonding, excess cement must be meticulously removed from the margin. Any leftover cement will harden and look dark, and over time, will lead to inflammation and recession.
The Fix: Rigorous attention to detail during preparation and bonding is key. The use of dental magnification and proper isolation (like a rubber dam) is essential. For existing failures, removal is complex. The old veneer must be carefully taken off, often requiring new preparation to correct the damaged margin. The new veneer must have a perfectly adapted, polished margin that sits flush with the tooth and is easy to clean.
4. The "Long-in-the-Tooth" Look: Gum Recession and Root Exposure
Veneers should enhance your smile, not accelerate its aging. When veneers are placed incorrectly, they can cause or exacerbate gum recession, making you look older and creating sensitivity.
What it looks like: The gums have receded since the veneers were placed, exposing the darker, often yellowish root surface of the tooth below the edge of the veneer. This creates a stark color and length contrast. The smile may look "long-toothed" and uneven. This is often accompanied by sensitivity to hot and cold.
Why it happens: Several factors converge here. Over-preparation into the dentin (the layer under enamel) can traumatize the tooth and lead to recession. Placing the veneer margin too far below the gumline (subgingival) irritates the periodontal tissue. Poor marginal fit, as described above, becomes a plaque trap, causing chronic inflammation (gingivitis) that destroys supporting gum tissue. Using a material with an aggressive, rough margin can also contribute.
The Fix: This is a serious complication. Prevention requires conservative preparation, staying primarily in enamel, and respecting biological widths. For existing recession, treatment is multi-stage. The bad veneers must be removed. Periodontal (gum) surgery may be needed to restore lost tissue and create a healthy, even gumline. Only then can new, properly designed veneers be placed with margins in a safe, cleanable position.
5. The "Bulky" or "Thick" Tooth: Poor Craftsmanship and Material Choice
A great veneer is indistinguishable from a natural tooth in thickness. When they look bulky, the illusion is completely broken.
What it looks like: The teeth appear unnaturally thick, especially from the sides and the biting edge. They may look like they are "floating" in front of the gums rather than emerging naturally from them. The patient may complain of a lisp or difficulty speaking clearly initially, as the veneers alter the tongue's space.
Why it happens: This is a lab and material issue. The dental lab may have used a low-quality porcelain that is less dense and requires more thickness for strength. More commonly, the dentist failed to provide the lab with a proper "reduction guide" or did not reduce the tooth sufficiently during preparation. The lab then makes the veneer thicker to compensate for strength, not realizing it will look bulky. Using the wrong material (e.g., a thick composite buildup instead of thin porcelain) for the situation also causes this.
The Fix: The solution is a full remake with a focus on minimal invasive dentistry. The new preparation should remove only the necessary enamel (often 0.3-0.7mm) to create space for a thin, strong porcelain veneer. The lab must be instructed to use high-strength, ultra-thin ceramic materials. A try-in is again vital to assess bulk before final bonding.
6. The "Chip and Crack" Saga: Material Failures and Bonding Errors
Veneers are strong, but they are not indestructible. Premature failure through chipping or cracking points to fundamental errors.
What it looks like: Small chips at the incisal edge (biting edge), cracks radiating from the surface, or entire veneers popping off. This can happen soon after placement or years later.
Why it happens:Chipping is often a material or design flaw. The veneer may be too thin in high-stress areas, or the lab may have used a weaker ceramic. A sharp, non-anatomical incisal edge (like a 90-degree corner instead of a rounded one) is a stress point. Cracking can occur from trauma or from underlying tooth flexure if the veneer is not properly bonded across its entire surface. Debonding (coming off) is almost always a bonding protocol failure: the tooth wasn't properly cleaned and etched, the veneer's internal surface wasn't correctly treated, or the bonding cement was improperly mixed or cured.
The Fix: Repairing a chipped veneer is often possible with composite bonding, but it may not be a perfect color match. A cracked veneer usually needs replacement. Debonded veneers can often be re-bonded if the tooth and veneer are undamaged, but this requires a flawless rebonding procedure. The root cause must be identified—was it a thin veneer, a sharp edge, or a bonding error?—to prevent recurrence.
7. The "Aftermath" of No Plan: Lack of Diagnostic Wax-Up and Mock-Up
This is the overarching cause of nearly all the failures above. Rushing into tooth preparation without a visual and functional plan is the single biggest predictor of bad veneers before and after outcomes.
What it looks like: The final result is a surprise to both the patient and the dentist. The shape, color, length, and smile line are all "guessed at" rather than meticulously planned. The patient’s facial features, lip dynamics, and gum symmetry were never properly analyzed.
Why it happens: The dentist may be inexperienced, pressured for time, or working with a low-cost lab that doesn't require or provide a diagnostic stage. The patient may have insisted on skipping the "extra steps" to save time or money. This is the equivalent of building a house without blueprints.
The Fix: This is 100% preventable. Never allow a dentist to prepare your teeth for veneers without first creating a diagnostic wax-up or digital mock-up and a physical try-in with a provisional (temporary) mock-up. This stage allows for adjustments based on how the proposed smile looks and functions on your face. It is the most critical step for a successful before and after transformation.
The Statistics and Stakes: Why This Matters
The American Academy of Cosmetic Dentistry (AACD) reports that over 1 in 3 adults are unhappy with their smile. This drives millions to seek cosmetic procedures like veneers annually. While the success rate for well-planned, expertly executed veneers is extremely high (often cited at 95%+ over 10 years), the rate of failure or dissatisfaction from poor work is a significant, though less publicized, problem. The cost of correcting bad veneers is financially and emotionally staggering. Patients often pay twice: once for the initial failure and again for the corrective work, which is typically more complex and expensive due to the need to undo damage. Beyond the wallet, the psychological toll is real. A smile is central to identity and social interaction. Living with a bad veneer before and after you never wanted can lead to social anxiety, depression, and a loss of self-esteem.
Your Action Plan: How to Guarantee a Good "After"
If you are considering veneers, your due diligence is your best defense. Here is your actionable checklist:
- Research Your Dentist Relentlessly: Don't just look for a "cosmetic dentist." Look for a dentist with accreditation or fellowship in cosmetic dentistry from a recognized body like the AACD. Ask to see dozens of before and after photos of their own work, specifically full-face smiles, not just close-ups of teeth. Ask for patient references.
- Demand the Diagnostic Process: Your first major red flag is a dentist who wants to prepare your teeth at the first visit. The process must be: Consultation > Digital Photos & Videos > Digital Smile Design > Diagnostic Wax-Up/Mock-Up > Physical Try-In of Mock-Up > Final Approval > Tooth Preparation. The try-in is non-negotiable.
- Understand the Materials: Ask about the dental lab. Is it a local, high-end cosmetic lab or a cheap overseas facility? You have the right to know. Ask about the specific porcelain system (e.g., e.max, lithium disilicate) being used and why.
- Communicate Your Desires (and Fears): Bring photos of smiles you like and, crucially, smiles you don't like. Be explicit about wanting a natural-looking result, not a "Hollywood white" set of Chiclets. Discuss your concerns about shape, length, and gum display.
- Get Everything in Writing: The treatment plan, cost, number of veneers, material, lab used, and the promise of a try-in should be part of your signed consent form.
Conclusion: Your Smile, Your Investment, Your Story
The journey of bad veneers before and after is a story of missed steps, poor communication, and compromised artistry. It’s a reminder that cosmetic dentistry is a true blend of medical science and artistic skill. The "after" you deserve is not a secret—it’s built on a foundation of transparency, meticulous planning, and a collaborative partnership with a qualified, ethical professional.
Do not let the fear of a bad outcome paralyze you. Let it instead empower you. Use this knowledge as your shield. A great before and after in cosmetic dentistry is a visible testament to patience, precision, and partnership. It’s a smile that looks like it was always yours—because it was designed with your unique face in mind from the very first diagnostic step. Choose wisely, plan thoroughly, and your smile transformation will be the success story you get to tell for a lifetime.