Enlarged Taste Buds On Tongue: Why They Swell And What It Means For Your Health
Have you ever caught a glimpse of your tongue in the mirror and noticed strange, red, swollen bumps that look unlike your usual tongue texture? That unsettling sensation of a "hairy" or "bumpy" tongue might lead you to a frantic internet search: "taste buds on tongue enlarged." It’s a common concern, and while it’s often harmless, understanding what’s really happening is key to peace of mind and proper oral care. Your tongue is a complex muscular organ, and its surface is a landscape of tiny structures called papillae, which house your taste buds. When these papillae become inflamed or irritated, they can appear significantly enlarged, red, or even white. This guide dives deep into the world of enlarged taste buds, exploring the surprising array of causes—from minor burns to underlying medical conditions—and providing clear, actionable steps to identify, soothe, and know when professional help is essential.
What Exactly Are Taste Buds and Papillae?
Before we explore why they swell, let's clarify the anatomy. Your tongue isn’t a smooth surface; it’s covered in thousands of tiny projections called papillae. There are four main types:
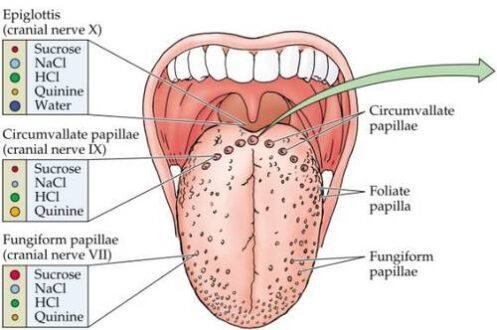
- Fungiform papillae: Mushroom-shaped, scattered across the tip and sides, each contains 1-8 taste buds.
- Foliate papillae: Leaf-like ridges on the sides toward the back.
- Circumvallate papillae: The largest, arranged in a V-shape near the back, each surrounded by a trench and containing hundreds of taste buds.
- Filiform papillae: The most numerous, but they do NOT contain taste buds. They are thin, conical, and provide the tongue's rough texture for gripping food.
Taste buds are the actual sensory organs—clusters of 50-150 specialized cells bundled inside the papillae (except filiform). They detect the five basic tastes: sweet, salty, sour, bitter, and umami. When people say their "taste buds are swollen," they are almost always referring to the enlargement of the papillae themselves, particularly the fungiform and circumvallate types, which become visibly prominent, red, and sometimes painful.
The Most Common Culprits Behind Enlarged Taste Buds
Physical Trauma: The #1 Offender
The most frequent cause of a suddenly enlarged taste bud is physical irritation. Your tongue is constantly in motion and contact with food, so it’s vulnerable.
- Biting Your Tongue: A accidental bite during eating or sleep can cause localized trauma, leading to inflammation and swelling of the papillae in that area.
- Burning: sipping scalding coffee, soup, or hot tea can literally cook the delicate surface cells. This is a classic cause of transient enlarged papillae, often accompanied by a raw, painful feeling.
- Sharp Foods: Chips, crusty bread, or fish bones can scrape or puncture the tongue surface.
- Dental Appliances: Braces, ill-fitting dentures, or even a sharp tooth edge can create constant friction.
Actionable Tip: After a burn or bite, rinse with cool salt water (1/4 tsp salt in 8 oz warm water) 2-3 times a day. This promotes healing, reduces inflammation, and prevents infection. Avoid acidic, spicy, or crunchy foods for 24-48 hours.
Irritants and Inflammatory Conditions
- Acidic or Spicy Foods: Citrus fruits, tomatoes, vinegar-based sauces, and chili peppers can chemically irritate the tongue, causing a temporary inflammatory response.
- Tobacco and Alcohol: Both are direct irritants to the oral mucosa. Smokers and frequent alcohol users often experience chronic irritation, leading to persistently enlarged or inflamed papillae.
- Allergic Reactions: Food allergies (e.g., to nuts, dairy, shellfish) or contact allergies to ingredients in toothpaste, mouthwash, or even certain metals in dental work can trigger localized swelling on the tongue.
- Geographic Tongue (Benign Migratory Glossitis): This is a fascinating, harmless condition where patches of papillae on the tongue surface temporarily disappear, leaving smooth, red "islands" with raised, white borders. The borders can appear as enlarged, inflamed papillae. The pattern changes location over weeks or months. It's often associated with psoriasis or stress but requires no treatment.
- Erythema Migrans: Similar to geographic tongue but the red patches are more uniform and lack the classic white borders. It's also benign.
Nutritional Deficiencies
Your tongue can be a window into your nutritional status. Deficiencies in key vitamins and minerals can manifest as changes in the tongue's appearance and texture, including swelling.
- Vitamin B12 Deficiency: Crucial for nerve function and cell production. A deficiency can cause glossitis (inflamed tongue), which presents as a smooth, red, swollen, and sometimes painful tongue. The papillae atrophy (shrink), but the overall inflammation can make adjacent papillae appear prominent.
- Folate (B9), Iron, and Niacin (B3) Deficiencies: These can also lead to glossitis and a swollen, beefy-red tongue appearance.
- Zinc Deficiency: Zinc is vital for cell growth and repair. A lack can impair taste sensation and cause tongue inflammation.
Practical Example: If you follow a restrictive diet (e.g., vegan without B12 supplementation, or very low-calorie), or have conditions like celiac disease or Crohn's that affect absorption, checking your B12 and iron levels is a wise step if you notice persistent tongue changes.
Infections: Viral, Bacterial, and Fungal
- Viral Infections: The herpes simplex virus (HSV-1), which causes cold sores, can also trigger herpetic glossitis, leading to painful, swollen, red areas on the tongue. Coxsackievirus (hand, foot, and mouth disease) causes distinctive blisters and sores on the tongue and mouth.
- Bacterial Infections: An overgrowth of bacteria in the mouth due to poor hygiene can lead to general inflammation.
- Fungal Infections (Oral Thrush): A Candida yeast overgrowth creates white, cottage-cheese-like patches that can be scraped off, sometimes leaving a red, inflamed, and tender surface underneath where papillae may appear swollen.
Systemic Medical Conditions
Sometimes, enlarged taste buds or tongue inflammation are symptoms of a broader health issue.
- Canker Sores (Aphthous Ulcers): These small, painful ulcers can appear on the sides or underside of the tongue. The tissue immediately around the ulcer often becomes red and inflamed, making nearby papillae look enlarged.
- Burning Mouth Syndrome (BMS): A chronic condition characterized by a burning, scalding sensation on the tongue (and sometimes lips, palate) with no visible cause. While the tongue may look normal, some patients exhibit mild papillae enlargement or atrophy. It's often linked to hormonal changes, nerve damage, or dry mouth.
- Autoimmune Diseases: Conditions like Sjögren's syndrome (causing severe dry mouth) or lupus can have oral manifestations, including tongue changes.
- Celiac Disease: Beyond malabsorption, gluten sensitivity can trigger an autoimmune response that affects the mouth, causing glossitis and canker sores.
- Diabetes: High blood sugar promotes bacterial and fungal growth, increasing the risk of oral infections and inflammation.
Medications and Medical Treatments
- Chemotherapy and Radiation: These cancer treatments are notorious for causing mucositis—severe inflammation and ulceration of the mucous membranes throughout the digestive tract, including the tongue. Papillae become massively swollen and painful.
- Certain Antibiotics: Can disrupt oral flora, leading to thrush.
- ACE Inhibitors (blood pressure meds): Can cause a dry cough and, less commonly, a swollen, tingling tongue (angioedema is a rare but serious side effect).
- Anticonvulsants and some Psychiatric Medications: May cause dry mouth or direct irritation.
Recognizing the Symptoms: More Than Just a Bump
An enlarged taste bud itself is a symptom. Pay attention to the full picture:
- Visual: Red, white, or pink swollen bumps. They might be isolated or in clusters. In geographic tongue, you'll see map-like red patches with white borders.
- Sensory: Tingling, burning, itching, or general tenderness on the tongue. A loss of taste (ageusia) or distorted taste (dysgeusia) can sometimes occur if the taste bud cells are damaged.
- Texture: The tongue may feel rough, "hairy," or sandpapery.
- Associated Symptoms: Fever, fatigue, or sores elsewhere in the mouth could indicate an infection. Dry mouth points to Sjögren's or medication side effects.
Red Flags That Warrant a Doctor's Visit:
- Swelling that does not improve after 1-2 weeks.
- Severe pain that interferes with eating, drinking, or speaking.
- Difficulty breathing or swallowing (signs of a serious allergic reaction or angioedema—seek emergency care).
- A persistent white patch that cannot be scraped off (could indicate leukoplakia, a precancerous condition).
- A lump or growth that feels hard and fixed.
- Numbness or loss of sensation in the tongue.
- Symptoms accompanied by unexplained weight loss, fatigue, or skin rashes.
Getting a Diagnosis: What to Expect at the Doctor or Dentist
If your enlarged taste buds are persistent or concerning, a professional evaluation is crucial. Here’s what typically happens:
- Medical & Dental History: Your provider will ask about diet, oral hygiene, medications, recent illnesses, allergies, and lifestyle habits (tobacco, alcohol).
- Physical Examination: A thorough inspection of your tongue, mouth, and throat. They may use a tongue depressor and good lighting to map any lesions.
- Diagnostic Tests:
- Swab or Scraping: To check for fungal (Candida) or bacterial infections.
- Blood Tests: To screen for nutritional deficiencies (B12, iron, folate), diabetes, or autoimmune markers.
- Biopsy: If a lesion looks suspicious, a small tissue sample may be taken for lab analysis to rule out serious conditions like oral cancer. This is the definitive diagnostic tool.
- Referral: You may be referred to an oral medicine specialist, an otolaryngologist (ENT), or a gastroenterologist if systemic disease is suspected.
Treatment and Management Strategies
Treatment is entirely dependent on the underlying cause. There is no one-size-fits-all cure for "enlarged taste buds."
Addressing the Root Cause
- Trauma/Irritation: Eliminate the source. Use a soft-bristled toothbrush, avoid irritating foods (acidic, spicy, hot), and ensure dental appliances fit correctly.
- Infections:
- Antifungal rinses or lozenges for thrush.
- Antiviral medication for severe herpes outbreaks.
- Antibiotics for specific bacterial infections.
- Nutritional Deficiencies: Supplementation under medical guidance (e.g., B12 injections or high-dose oral supplements, iron pills).
- Systemic Conditions: Managing the primary disease (e.g., controlling diabetes with an endocrinologist, treating celiac disease with a strict gluten-free diet) will often resolve the oral symptoms.
- Medication-Related: Discuss alternatives with your prescribing doctor. For dry mouth, saliva substitutes and stimulants (like sugar-free gum) can help.
Symptomatic Relief and Home Care
While you address the cause, these measures can soothe discomfort:
- Salt Water Rinses: As mentioned, a gold standard for reducing inflammation and promoting healing.
- Cool Foods and Drinks: Yogurt, smoothies, chilled applesauce. Avoid anything hot.
- Honey: A natural antimicrobial and anti-inflammatory. A teaspoon can coat and soothe.
- Avoid Alcohol-Based Mouthwashes: They are drying and irritating. Opt for an alcohol-free, gentle formula or a simple salt water rinse.
- Stay Hydrated: A well-hydrated mouth is more resilient. Sip water throughout the day.
- Good Oral Hygiene: Gently brush your tongue with a soft toothbrush or a silicone tongue scraper from back to front to remove debris and bacteria. Don't scrub aggressively.
When to Consider Professional Procedures
For persistent, bothersome geographic tongue or Burning Mouth Syndrome with no clear cure, management is key:
- Topical Corticosteroids: A dentist or doctor may prescribe a mild steroid rinse or paste to reduce inflammation in severe cases of glossitis or geographic tongue.
- Anesthetic Rinses: For BMS, rinses containing lidocaine can temporarily numb the tongue for pain relief.
- Cognitive Behavioral Therapy (CBT): Proven effective for BMS, as it helps manage the chronic pain perception and associated anxiety.
Prevention: Cultivating a Healthy Tongue Ecosystem
An ounce of prevention is worth a pound of cure. Protect your tongue with these habits:
- Mindful Eating: Let hot food and drinks cool. Chew slowly to avoid bites.
- Optimal Oral Hygiene: Brush twice daily, floss, and clean your tongue gently. This controls bacterial load.
- Balanced Diet: Ensure adequate intake of B vitamins, iron, and zinc. Include leafy greens, lean meats, legumes, nuts, and whole grains.
- Hydration: Drink plenty of water. Limit dehydrating drinks like coffee and alcohol.
- Regular Dental Check-ups: Your dentist is often the first to spot oral changes. Get cleanings every six months.
- Manage Stress: Stress is a known trigger for geographic tongue and canker sores. Incorporate stress-reduction techniques like meditation, yoga, or regular exercise.
- Quit Tobacco and Limit Alcohol: These are major irritants to the oral mucosa.
Frequently Asked Questions About Enlarged Taste Buds
Q: Can enlarged taste buds affect my sense of taste?
A: Yes, but usually temporarily. If the taste bud cells themselves are damaged (from a burn or infection), your taste perception in that immediate area may be dulled or distorted until new cells regenerate (taste buds turnover every 10-14 days). Widespread inflammation (glossitis) can dull overall taste.
Q: How long does it take for an enlarged taste bud to go away?
A: It depends entirely on the cause. A burn or minor bite may resolve in 3-7 days. Geographic tongue patches can last weeks to months before moving. Deficiencies or systemic conditions may take weeks to months of treatment to see improvement.
Q: Is it contagious?
A: The condition of having enlarged papillae itself is not contagious. However, if it's caused by a viral infection (like herpes) or a fungal overgrowth (thush), the underlying infection can be contagious.
Q: Should I scrape my tongue if my taste buds are swollen?
A: Be extremely gentle. If you use a tongue scraper, use light pressure and stop if it's painful. A soft toothbrush is often a safer option. Aggressive scraping can worsen trauma and inflammation.
Q: Can stress really cause this?
A: Absolutely. Stress is a major trigger for canker sores and geographic tongue flares. It can also exacerbate conditions like Burning Mouth Syndrome. The mind-body connection in oral health is very real.
Q: Are enlarged taste buds a sign of cancer?
A: Not usually. Most causes are benign. However, any persistent, non-healing ulcer, lump, or red/white patch that doesn't resolve in 2-3 weeks should be evaluated by a professional to rule out oral cancer. Do not ignore persistent changes.
Conclusion: Listening to Your Tongue's Signals
Enlarged taste buds on the tongue are overwhelmingly a sign of local irritation, minor trauma, or a nutritional imbalance—issues that are often simple to resolve. Yet, your tongue's surface is also a dynamic canvas that can reflect deeper systemic health, from vitamin deficiencies to autoimmune disorders. The key is observation and context. Note the duration, associated symptoms, and your recent lifestyle or health changes. For the vast majority of cases stemming from a burnt pizza bite or a spicy curry night, simple home care and patience are all you need. However, when swelling is persistent, painful, or accompanied by other unexplained symptoms, it’s your body’s signal to seek a professional opinion. Don’t dismiss a chronically altered tongue. By understanding the potential causes—from the mundane to the medically significant—you empower yourself to take appropriate action, ensuring your tongue remains not just a map of papillae, but a clear indicator of your overall well-being.