What Does A Cavity Feel Like? Your Complete Guide To Tooth Decay Sensations
Have you ever suddenly felt a sharp twinge in your tooth while sipping something cold, or noticed a new spot that looks different on your enamel? You might have wondered, what does a cavity feel like? It’s a common question, and the answer isn’t always simple. The sensation can range from completely unnoticed to excruciating pain, depending entirely on how far the decay has progressed. Understanding these feelings is your first line of defense in catching tooth decay early and preventing a small problem from becoming a dental emergency. This guide will walk you through every possible sensation, from the earliest warning signs to the severe pain of an advanced abscess, so you know exactly when to pick up the phone and call your dentist.
The Spectrum of Sensations: It’s Not Always Pain
One of the most crucial things to understand about cavities is that they don’t always hurt. In fact, the earliest stage of decay, which affects only the hard, outer enamel, is often completely asymptomatic. This is why regular dental checkups and cleanings are non-negotiable; your dentist can spot decay you can’t feel or see. As the decay progresses and breaches the enamel to reach the softer dentin layer underneath, sensations begin to emerge. The feeling is typically described as a localized discomfort, sensitivity, or ache centered on one specific tooth. It’s rarely a vague, whole-mouth pain. The type and intensity of the feeling depend on what layer of the tooth is affected and whether the decay has reached the nerve.
Common Early-Stage Sensations: The Warning Signs
When decay first moves beyond the enamel into the dentin, you might experience:
- Increased Sensitivity: A sharp, fleeting pain or discomfort when your tooth comes into contact with hot, cold, sweet, or acidic foods and drinks. This is because dentin contains thousands of microscopic tubules that lead directly to the nerve of the tooth. Once the protective enamel is compromised, stimuli travel more easily to the pulp.
- Staining and Texture Changes: You might visually notice a white spot on the tooth (a sign of mineral loss) or a brown, black, or gray stain that looks like a hole or pit. You may also run your tongue over it and feel a rough, uneven, or "sticky" spot where the enamel has softened and broken down.
- Mild, Intermittent Discomfort: A vague ache or pressure in the area that comes and goes, often after eating. It might feel like something is "caught" in your tooth or like a dull throbbing that you can almost ignore.
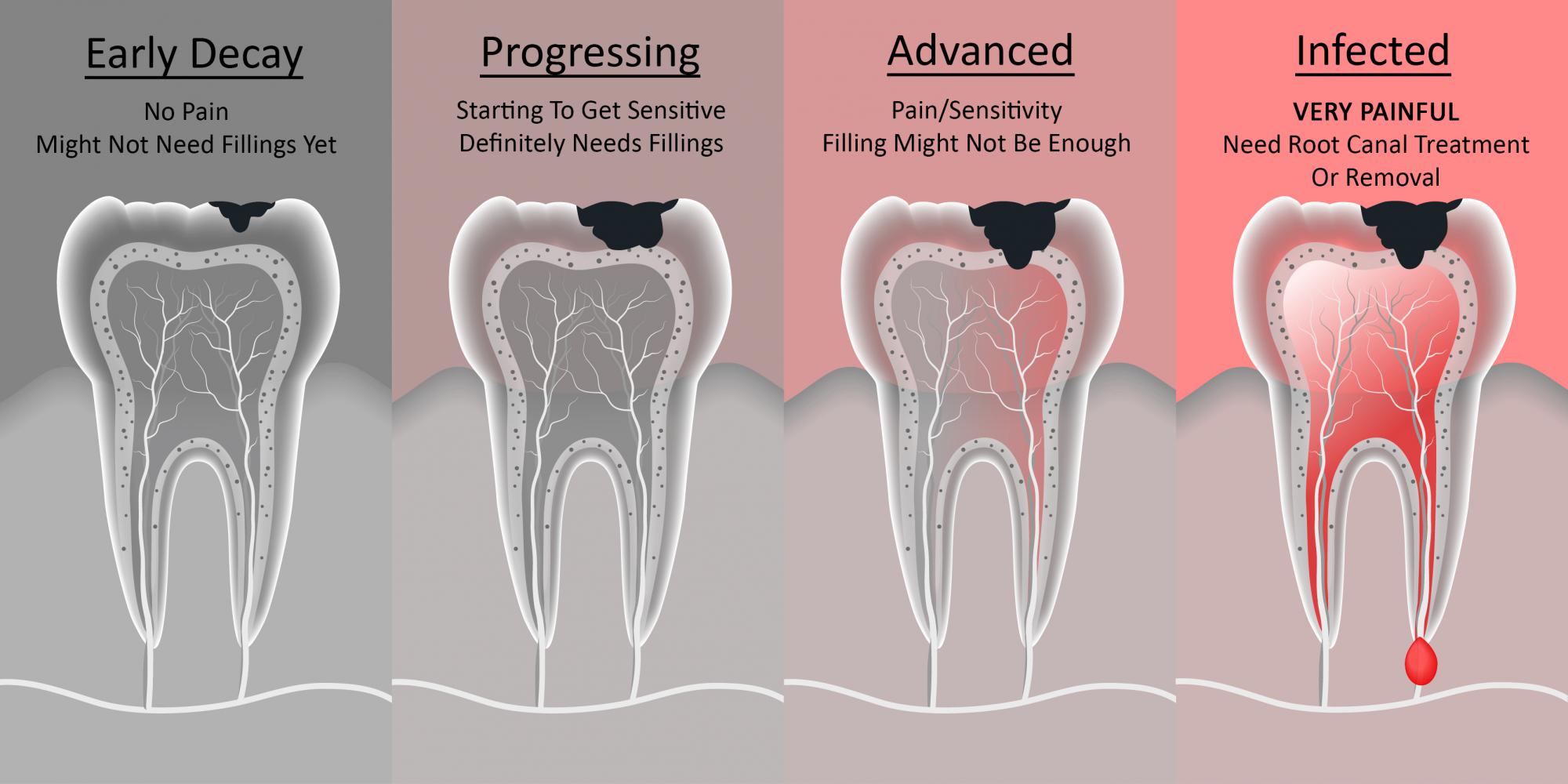
The Progression: How Decay Feels at Each Stage
To understand what a cavity feels like, you need to know the anatomy of a tooth and how decay travels through it. Think of it like an invasion: the enemy (bacteria and acid) slowly breaches the outer walls (enamel), then the inner chambers (dentin), and finally the central command center (the pulp).
Stage 1: Enamel Decay (The Silent Stage)
- Feeling:None. This is the critical point. The enamel has no nerves or blood vessels. It can be demineralized and even develop a small cavity without you feeling a thing. This is why the CDC reports that roughly 1 in 4 adults has untreated tooth decay—it’s often hiding silently.
- What’s Happening: Bacteria in plaque metabolize sugars from your diet and produce acid. This acid leaches minerals (calcium and phosphate) from the enamel, creating a weak, porous area. If caught here, the process is reversible with fluoride and improved oral hygiene.
Stage 2: Dentin Decay (The Sensitivity Stage)
- Feeling:Sharp sensitivity to temperature and sweets, mild ache.
- What’s Happening: Once the acid breaks through the enamel, it hits the dentin. Dentin is much softer and contains those tiny tubules connected to the pulp. Now, hot, cold, and sweet stimuli travel directly to the nerve, causing that characteristic zing or shock of pain. The decay spreads faster through dentin. The feeling is now tooth-specific and triggered.
Stage 3: Pulp Involvement (The Pain Stage)
- Feeling:Constant, throbbing, severe pain; spontaneous pain; pain that wakes you up at night.
- What’s Happening: The decay has now reached the innermost pulp chamber, which houses the tooth’s nerve and blood supply. The bacteria infect the pulp, causing inflammation (pulpitis). The pulp is enclosed in a rigid shell, so as it swells, pressure builds on the nerve, causing intense, unrelenting pain. This pain often becomes spontaneous (not just triggered by something) and can be a deep, throbbing ache. At this point, a root canal is typically necessary to save the tooth.
Stage 4: Abscess Formation (The Emergency Stage)
- Feeling:Extreme, unrelenting pain; swelling in the gum or face; fever; a bad taste in the mouth.
- What’s Happening: The infected pulp dies, and the infection spreads out the tip of the tooth root into the surrounding bone, forming an abscess (a pocket of pus). This is a serious medical condition. The pain is often worse when you lie down due to increased blood flow to the area. You might see a pimple-like swelling (fistula) on the gum above the tooth, which can drain pus. This requires immediate dental attention, often antibiotics and a root canal or extraction.
Different Types of Cavity Pain: What They Mean
Not all cavity pain feels the same. The character of the pain can give you clues about what’s happening inside.
- Sharp, Shooting Pain: This is classic for sensitivity due to exposed dentin. It’s fast, electric, and stops as soon as the stimulus (cold drink, sweet food) is removed. It points to a reversible issue if caught early.
- Dull, Throbbing, or Aching Pain: This indicates inflammation is reaching the pulp. The pain is more constant and pressure-like. It might linger after the trigger is gone. This suggests irreversible pulpitis and the need for urgent care.
- Pain When Biting or Chewing: This can happen with larger cavities that have weakened the tooth structure, causing a cracked tooth syndrome or an abscess. The pain is a sharp, focused jab upon release of the bite.
- Spontaneous Pain (No Trigger): Pain that comes out of nowhere, often at night, is a major red flag for pulp damage. The nerve is inflamed and firing on its own.
- Pain That Radiates: Sometimes, you can’t pinpoint the exact tooth. The pain seems to spread to your jaw, ear, or head. This is common with lower jaw abscesses or severe pulpitis.
The "Tongue Test" and Other Self-Checks
While not a substitute for a dentist, you can gently explore (with clean hands!) a suspicious spot with your tongue. A cavity often feels rough, sticky, or like a little pit or hole compared to the smooth, hard surface of healthy enamel. You might also notice food getting "stuck" in a particular spot more often. A discolored spot (brown/black) that looks like a stain but is actually part of the tooth structure is a visual clue.
Hidden Cavities: The Ones You Can’t See or Feel
Here’s a scary truth: some of the most dangerous cavities are the ones you have no idea exist. These are often:
- Interproximal Cavities (Between Teeth): These form between your teeth where your brush can’t reach. They start as a small demineralization between the enamel walls and can quickly tunnel into the dentin and pulp without any visual sign until they are large. You might not feel sensitivity until they are quite advanced. This is why flossing is absolutely critical—it disrupts plaque in these areas.
- Root Cavities: As gums recede with age or gum disease, the softer root surface (cementum) becomes exposed. This area is much more susceptible to rapid decay. These can progress quickly and are often found in older adults.
- Cavities Under Old Fillings or Crowns: Over time, the seal around a filling can break down, allowing bacteria and acid to leak underneath and cause new decay. This "secondary decay" is often invisible to the naked eye and may only be detected by a dentist via X-ray or exploration.
Prevention: The Only Way to Avoid the Feeling
The best way to know what a cavity feels like is to never find out. Prevention is infinitely easier, cheaper, and less painful than treatment. Here is your actionable defense plan:
- Master Your Brushing: Brush for two minutes, twice a day, with a fluoride toothpaste. Use a soft-bristled brush and make small circular motions to clean at the gum line. Consider an electric toothbrush for superior plaque removal.
- Floss Daily, Without Exception: Floss is your #1 weapon against hidden interproximal cavities. Use about 18 inches of floss, curve it around each tooth in a C-shape, and slide it gently under the gumline.
- Limit Sugary and Acidic Attacks: Bacteria love sugar. Every time you eat or drink something sugary or acidic (soda, juice, sports drinks, candy), your mouth’s pH drops, creating an acid attack that lasts 20-30 minutes. Sipping on these drinks all day is the worst thing you can do—it’s a constant acid bath. Drink water instead, and if you do have a treat, consume it with a meal and rinse with water afterward.
- Use Additional Fluoride: Ask your dentist about supplemental fluoride treatments, fluoride rinses, or prescription-strength toothpaste if you are at high risk.
- See Your Dentist Regularly:Every six months for a cleaning and exam is the standard. Your hygienist removes hardened plaque (tartar) you can’t, and your dentist uses X-rays and visual tools to find decay in its earliest, invisible stages.
What to Do If You Suspect a Cavity
Do not wait. If you experience any persistent sensitivity, pain, or see a visible spot, schedule a dental appointment immediately. Early-stage decay might be treatable with a simple fluoride varnish or a small, painless filling. Waiting turns a $100 filling into a $1,000+ root canal and crown, or worse, a tooth extraction.
Conclusion: Listen to Your Mouth, Trust Your Dentist
So, what does a cavity feel like? The answer is a spectrum—from absolutely nothing, to a fleeting sensitivity, to a debilitating, sleepless agony. The feeling is your mouth’s alarm system, alerting you that the battle against plaque acid is being lost. The most important takeaway is this: the absence of pain does not mean the absence of disease. You cannot diagnose a cavity by feel alone. The only way to truly know the health of your teeth is through the professional assessment of a dentist using visual exams, explorers, and X-rays. Your role is to be vigilant for any changes in sensation or appearance, maintain an impeccable daily oral hygiene routine, and never skip your dental appointments. By understanding these sensations and acting swiftly, you protect not just your teeth, but your overall health, your smile, and your peace of mind. If in doubt, get it checked out—your future self will thank you.