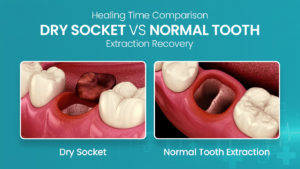
Dry Socket Vs Normal Healing: Visual Guide To Tooth Extraction Recovery
Have you ever found yourself staring at your healing socket after a tooth extraction, wondering if what you see is normal or a sign of trouble? The internet is flooded with pictures of dry socket vs normal healing, but making sense of them can be confusing and even alarming. Understanding the visual cues of proper recovery versus the warning signs of a complication like dry socket is crucial for every patient. This comprehensive guide will walk you through the distinct visual and symptomatic differences, empowering you to monitor your healing with confidence and know exactly when to contact your dentist.
Understanding the Basics: What Happens After a Tooth Extraction?
Before diving into visual comparisons, it's essential to understand the two very different healing processes we're examining. A normal extraction healing follows a predictable, biological sequence where your body efficiently repairs the wound. In contrast, dry socket (alveolar osteitis) is a painful complication that disrupts this natural progression. Knowing the fundamental mechanics of each process provides the foundation for accurately interpreting any pictures or your own recovery.
The Normal Healing Timeline: A Biological Masterpiece
After a tooth is removed, your body immediately springs into action. The first 24 hours are marked by blood clot formation within the empty socket. This blood clot is not just a byproduct; it's the critical foundation for healing. It protects the underlying bone and nerve endings, stops bleeding, and serves as a scaffold for new tissue growth. Over the next few days, this clot is gradually replaced by granulation tissue—a soft, pinkish, fleshy material that looks similar to the inside of your cheek. This tissue is rich in blood vessels and collagen, paving the way for bone and gum tissue to regenerate. By the end of the first week, the socket begins to shrink and fill in. Complete bone remodeling can take several months, but the initial soft tissue closure typically occurs within 2-3 weeks, leaving a smooth, healed gum line.
What is Dry Socket? A Disruption of the Process
Dry socket occurs when this crucial blood clot either fails to form properly, dissolves too early, or is dislodged from the socket. Without the protective clot, the bare bone and nerve endings in the socket are exposed to the oral environment—air, food particles, bacteria, and temperature changes. This exposure leads to intense, often radiating pain that typically begins 2-4 days after the extraction. The term "dry socket" is literal; the socket appears dry, often with a visible, darkish bone at the bottom, rather than being filled with healthy, moist granulation tissue. It's a localized inflammatory response, not an infection, though it can become secondarily infected.
Visual Comparison: Pictures of Dry Socket vs Normal Healing
While professional diagnosis is always required, visual inspection (with a flashlight and mirror, never poking at the site) can offer clues. Here’s a breakdown of what you might see in comparative pictures and in your own mouth.
Normal Healing: What to Expect to See
In pictures of normal post-extraction sites, the progression is clear:
- Days 1-3: The socket is filled with a dark red or maroon blood clot. It may look like a dark plug. The surrounding gum is swollen, pink, and possibly bruised.
- Days 4-7: The blood clot is being overgrown by granulation tissue. This tissue is bright red or deep pink, moist, and has a somewhat granular or "bumpy" appearance, like raw meat but pinker. The socket opening starts to look smaller as the tissue rises.
- Week 2+: The granulation tissue matures. The socket becomes much shallower, filled with smoother, pinker gum tissue. The hole is visibly closing. There should be no exposed bone, no foul odor, and only mild, residual tenderness.
Dry Socket: The Tell-Tale Visual Signs
Pictures of dry socket present a starkly different picture:
- The Socket Appears Empty or "Dry": This is the hallmark. Instead of a moist, red/pink plug, you see a dark, empty hole. The depth may be surprising.
- Exposed Bone: At the bottom of the socket, you can often see a smooth, yellowish-white or grayish piece of bone. This is the tooth's alveolar socket wall. It looks dry and may have a shiny or creamy appearance.
- Lack of Granulation Tissue: There is an absence of the healthy, red, fleshy granulation tissue that should be filling the space.
- Possible Grayish Discoloration: The tissue at the socket's edges might look grayish or dusky, indicating poor blood supply and necrosis (tissue death).
- Debris: Food particles or debris can be easily seen lodged in the socket because there's no clot to trap them away from the bone.
Important Disclaimer:Self-diagnosis via pictures is extremely risky. Many other conditions, like a normal but slow-healing socket, a localized infection, or even a bony fragment, can mimic these visuals. Always consult your oral surgeon or dentist for an accurate diagnosis.
Beyond the Picture: Symptom Comparison
Visuals are just one part of the equation. The symptom profile is often the most reliable indicator.
Normal Healing Symptoms
- Pain: Significant pain for the first 2-3 days, managed effectively with prescribed or OTC pain medication. Pain should steadily decrease each day.
- Swelling: Peaks around day 2-3 and then subsides.
- Bleeding: Minor oozing or spotting for the first 24 hours is normal. Active bleeding should stop with pressure.
- Odor/Taste: No persistent foul odor or bad taste. A slight metallic taste from the clot is normal initially.
- Overall Feeling: Gradual improvement. You should feel noticeably better each passing day after the initial peak.
Dry Socket Symptoms
- Pain:Severe, throbbing, and radiating pain that starts or worsens 2-4 days post-extraction. It often radiates to the ear, temple, neck, or other teeth on the same side. Pain is not relieved by typical pain medication and may even wake you at night.
- Visible Bone: As described above.
- Odor/Taste: A persistent, foul odor and a bad, salty or putrid taste in the mouth that does not go away with rinsing.
- Lack of Anesthesia Effectiveness: If you had a local anesthetic, the numbness should have worn off long ago. The pain of dry socket is not masked by lingering anesthesia.
The Critical Factor: Timeline
The timeline is a key differentiator that pictures alone can't convey.
- Normal Healing: The most uncomfortable phase is the first 72 hours. By day 4, pain and swelling should be on a clear downward trend.
- Dry Socket: The pain intensifies after the initial 2-4 days. If you feel relatively okay on day 2 and then experience a sharp, worsening pain on day 4 or 5, it's a major red flag.
Risk Factors & Prevention: Can You Avoid Seeing Those Dry Socket Pictures?
Certain factors increase your risk of developing dry socket. Knowing them allows you to take proactive steps.
- Smoking & Tobacco Use: The #1 risk factor. The suction motion and chemicals in smoke can dislodge the clot.
- Oral Contraceptives: Higher estrogen levels may increase risk.
- Previous Dry Socket History: If you've had one, you're more likely to have another.
- Traumatic or Complicated Extraction: More surgical intervention means more disturbance to the clot.
- Poor Oral Hygiene (Post-Op): But also, over-zealous rinsing/spitting in the first 24 hours.
- Age: Higher incidence in people over 30.
Actionable Prevention Tips
- Don't Smoke: Avoid for at least 72 hours after extraction, preferably a full week. Use nicotine patches if needed.
- Avoid Suction: No straws, no vigorous rinsing, no spitting for the first 24 hours. Gently tilt your head to let liquids fall from your mouth.
- Soft Diet: Stick to soft foods (yogurt, applesauce, mashed potatoes) for several days. Avoid crunchy, sticky, or small-seeded foods (like sesame seeds) that can lodge in the socket.
- Oral Hygiene: Gently brush teeth away from the extraction site. Start rinsing with a prescribed antimicrobial mouthwash or warm salt water only after 24 hours, and do so gently.
- Follow Instructions: Adhere strictly to your dentist's post-operative guidelines. They know the specifics of your extraction.
When to Seek Immediate Help: Don't Rely on Google Images
While comparing pictures can be educational, it is not a substitute for professional medical advice. You should call your dentist or oral surgeon immediately if you experience:
- Severe or worsening pain 3+ days after extraction.
- A foul odor or bad taste that persists.
- You can see what appears to be exposed bone in the socket.
- The pain is not controlled with your prescribed medication.
- You have a fever, swelling that increases after day 3, or pus (these may indicate infection, not just dry socket).
Treatment for dry socket is straightforward but requires a dental visit. The dentist will gently clean the socket, place a medicated dressing (often containing analgesic and antiseptic ingredients) into the socket to protect it and relieve pain, and may prescribe a stronger pain medication or antibiotics. With treatment, significant pain relief is often felt within hours.
Frequently Asked Questions About Dry Socket vs Normal Healing
Q: Can I take a picture of my own socket to compare?
A: You can, but with extreme caution. Use a flashlight and a clean spoon to gently pull your cheek away for a clear view. Do not touch the socket with your fingers or the spoon. The goal is to see, not to probe. Remember, lighting and angle dramatically affect what you see. Your dentist's professional assessment is always superior.
Q: Is a white or gray color in the socket always dry socket?
A: No. A white or yellowish film over a healing socket in the first week can sometimes be a layer of fibrin (part of the normal clotting process) or a small piece of food debris. The key is the context: is there severe pain and foul odor associated with it? If yes, it's concerning. If no, it may be normal.
Q: How long does it take for a dry socket to heal after treatment?
A: With proper treatment (dressing changes every few days), pain usually subsides significantly within a few days to a week. The socket will then begin to fill with new granulation tissue and heal, a process that takes 2-4 weeks from the initial extraction date.
Q: Can normal healing look "ugly" or scary?
A: Absolutely. The early granulation tissue can look red, raw, and uneven. There might be small bone spicules (tiny, sharp bone fragments) that work their way to the surface—this is usually normal unless accompanied by severe pain. Swelling and bruising can be dramatic but are often normal. The absence of severe, worsening pain is the most reassuring sign.
Conclusion: Trust the Process, But Trust Your Dentist More
While the internet offers countless pictures of dry socket vs normal healing, your most valuable tools are knowledge of the symptoms and a direct line to your dental professional. Normal healing, though sometimes uncomfortable and visually surprising, follows a path of steady improvement. Dry socket is defined by a specific, worsening pain pattern and a distinct visual of an empty, bone-exposed socket. Your best strategy is proactive prevention and attentive monitoring. If your recovery deviates from the expected path of steady improvement, especially regarding pain, do not hesitate to reach out. A quick call and a professional look can mean the difference between a week of unnecessary agony and a swift return to comfort. Your oral health is worth that expert eye.