7 Week Pregnancy Sonography: Your First Glimpse Of Baby's World
Can you really see your baby’s heartbeat at just 7 weeks? For many expectant parents, the first ultrasound scan is a moment of awe and relief, transforming the abstract idea of pregnancy into a tangible, flickering reality on a screen. The 7 week pregnancy sonography, often referred to as an early pregnancy or dating scan, is a pivotal milestone. It’s not just about a cute picture; it’s a critical diagnostic tool that confirms the pregnancy is viable, located correctly, and progressing as expected. This comprehensive guide will walk you through every aspect of this essential appointment, from the science behind the scan to what you’ll actually see and feel.
This early ultrasound serves as the foundational check-up for your pregnancy journey. It provides your healthcare provider with vital information to calculate your due date accurately and establish a baseline for your baby’s growth. For you, it’s the first real connection, a moment where anxiety can transform into joyful anticipation. Understanding what happens during a 7 week ultrasound, what the sonographer is looking for, and how to prepare can make this experience even more meaningful and less stressful. Let’s dive deep into the world of early prenatal imaging.
Confirming a Viable Intrauterine Pregnancy
The primary goal of a 7 week sonography is to confirm that the pregnancy is developing inside the uterus, where it belongs. This is the first and most crucial step in ensuring a healthy pregnancy. The sonographer will use a transvaginal ultrasound (TVS), which provides a clearer image at this early stage than an abdominal scan. A small, wand-like probe is gently inserted into the vagina, offering a close-up view of the pelvic organs without the need for a full bladder, though some fluid may still be required.
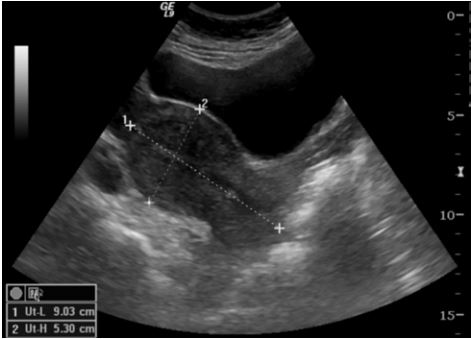
During this part of the scan, the technician will locate the gestational sac. This is the fluid-filled structure that houses the developing embryo. Seeing a gestational sac within the uterine cavity is the first positive sign. Its size, shape, and location are meticulously measured and noted. An irregularly shaped sac or one positioned low in the uterus might warrant closer monitoring, but often, variations are normal. The confirmation that the pregnancy is intrauterine immediately rules out the risk of an ectopic pregnancy—a serious condition where the embryo implants outside the uterus, most commonly in a fallopian tube. This early confirmation provides immense peace of mind.
The Importance of the Gestational Sac Measurement
The mean sac diameter (MSD) is a key measurement taken at this stage. It helps verify the gestational age, especially if your last menstrual period (LMP) is uncertain. The sac grows predictably, and its size in millimeters should roughly correspond to your week of pregnancy. For instance, at 7 weeks, the gestational sac typically measures between 16-24 mm. This measurement, combined with other findings, helps your doctor affirm or adjust your estimated due date (EDD), which is crucial for all future prenatal planning and testing timelines.
Detecting the Fetal Pole and Cardiac Activity
One of the most magical moments of a 7 week pregnancy scan is the potential to see the fetal pole—the first visible sign of the developing embryo—and, even more remarkably, to detect its tiny, rapid heartbeat. The fetal pole is a thickening on the edge of the gestational sac that will eventually develop into your baby. By 7 weeks, it is usually visible in a viable pregnancy.
More importantly, this is the stage where a fetal heartbeat can often be detected. Using Doppler technology, the ultrasound machine picks up the movement of blood through the embryonic heart. You’ll likely hear a fast, galloping sound—a rate between 90 and 110 beats per minute (bpm) is typical at this age. Seeing that flickering light on the screen and hearing that strong, steady beat is an emotional milestone for parents. Studies suggest that by 7 weeks gestation, a fetal heartbeat is detectable in over 90% of confirmed singleton pregnancies when a transvaginal ultrasound is used.
Understanding Heartbeat Variability
It’s important to understand that a detectable heartbeat at 7 weeks is a very positive sign, but its absence doesn’t always mean the pregnancy has failed. Factors like a slightly later conception date than calculated, a tilted uterus, or technical limitations can sometimes make it difficult to see. Your doctor will consider the size of the gestational sac and fetal pole. If the sac is large (e.g., >25 mm MSD) but no fetal pole or heartbeat is seen, it may indicate a blighted ovum (anembryonic pregnancy) or a missed miscarriage. However, if everything is measuring appropriately for 7 weeks, they will likely recommend a follow-up scan in 7-10 days to reassess. This cautious approach avoids premature conclusions.
Checking for Multiple Pregnancies
A 7 week ultrasound is also the earliest and most reliable method for identifying a multiple pregnancy, such as twins or triplets. The sonographer will carefully examine the gestational sac(s). In the case of twins, there are two primary configurations:
- Dizygotic (Fraternal) Twins: Each twin has its own separate gestational sac, its own fetal pole, and its own placenta (dichorionic diamniotic). This is the most common type and is visible as two distinct sacs very early on.
- Monozygotic (Identical) Twins: Depending on when the single fertilized egg splits, the twins may share a placenta (monochorionic). At 7 weeks, this can sometimes be indicated if there is a single gestational sac with two fetal poles ("monoamniotic" if they share the same amniotic sac, which is rarer) or two sacs that are very close together with a thin, shared membrane.
Identifying multiples this early is critical for prenatal care. Multiple pregnancies are considered higher risk and require more frequent monitoring for conditions like twin-to-twin transfusion syndrome (TTTS) in monochorionic twins, preterm labor, and gestational hypertension. Knowing the chorionicity (number of placentas) at this early stage dictates the entire follow-up schedule for your pregnancy.
The "Lambda" and "T" Signs
Your sonographer will look for specific markers to determine chorionicity. The lambda sign (or "twin peak sign")—a triangular, pointed projection of the intertwin membrane where it meets the placenta—indicates a dichorionic pregnancy (separate placentas). A "T" sign, where the membrane joins the placenta in a straight line, suggests a monochorionic pregnancy (shared placenta). Spotting these subtle signs at 7 weeks sets the stage for specialized care.
Assessing the Yolk Sac and Early Development
Alongside the gestational sac and fetal pole, the yolk sac is another vital structure visible on a 7 week ultrasound. This small, circular, echo-free circle is attached to the fetal pole and plays a crucial role in early embryonic development. It is the primary source of nutrients for the embryo before the placenta is fully formed and functional. It is also the site of early blood cell production.
The presence, size, and shape of the yolk sac are important indicators of pregnancy health. A yolk sac should be visible when the mean sac diameter reaches 5-6 mm. A normally sized yolk sac (typically 3-6 mm at 7 weeks) is a reassuring sign. An abnormally large yolk sac (over 6 mm) or an irregularly shaped one can sometimes be associated with an increased risk of miscarriage or chromosomal abnormalities, though it is not a definitive diagnostic marker on its own. Your doctor will note this as part of the overall picture.
The Journey from Yolk Sac to Placenta
It’s fascinating to track this transition. The yolk sac begins to shrink and is eventually incorporated into the developing umbilical cord and gastrointestinal tract as the placenta takes over the nourishing role around weeks 10-12. Seeing this tiny, vital structure on the scan at 7 weeks is a testament to the intricate and rapid biological processes already at work in your body.
Ruling Out Ectopic Pregnancy and Other Concerns
One of the most critical medical functions of an early 7 week sonography is to definitively rule out an ectopic pregnancy. This is a life-threatening condition where the fertilized egg implants outside the uterine cavity, most commonly in a fallopian tube. A transvaginal ultrasound is the gold standard for this diagnosis. The sonographer will meticulously sweep through the uterus and adnexal areas (where the ovaries and tubes are).
If no intrauterine pregnancy is seen, but there is a suspicious mass, fluid in the abdomen (indicating possible rupture), or a positive pregnancy test, it becomes an urgent situation. The absence of a yolk sac or fetal pole within a gestational sac that is larger than 20-25 mm (the "empty sac" sign) can also suggest a non-viable intrauterine pregnancy or an early ectopic. This scan, therefore, is a powerful tool for ensuring your immediate physical safety.
Recognizing Adnexal Masses
Sometimes, a small cyst or the corpus luteum (the structure that produced progesterone after ovulation) can be seen near the ovary. The sonographer is trained to distinguish these normal structures from a potential ectopic gestation. Clear visualization of the uterus empty of a pregnancy, combined with pelvic pain or bleeding, would lead to immediate medical follow-up. The peace of mind gained from a normal, intrauterine finding at 7 weeks cannot be overstated.
Understanding the Limitations of a 7 Week Scan
While a 7 week pregnancy ultrasound is incredibly informative, it has inherent limitations due to the tiny size of the embryo. It is not a detailed anatomy scan. Structures like limbs, facial features, or internal organs are not yet sufficiently developed to be assessed. The primary purpose is viability, location, and dating, not a full physical survey. Parents sometimes have unrealistic expectations, hoping to see a fully formed baby, but at this stage, the embryo is only about the size of a blueberry or a lentil (approximately 0.5 inches or 1.2 cm long).
The image will likely show a tiny flicker (the heartbeat) next to a small yolk sac within a larger dark gestational sac. You may see the beginning of the neural tube, which will become the brain and spine, as a subtle white line. It’s a glimpse of potential, not a detailed portrait. Understanding this helps manage expectations and allows you to appreciate the profound information that is available: the confirmation of life and its correct location.
What "Normal" Looks Like at 7 Weeks
A typical report might read: "Intrauterine pregnancy consistent with 7 weeks gestation. Gestational sac measuring 20 mm. Fetal pole identified with cardiac activity of 110 bpm. Yolk sac present. No adnexal masses." This is the gold standard. Variations can occur, and your provider will interpret the findings in the context of your specific health history and symptoms.
How to Prepare and What to Expect During the Scan
Preparation for a 7 week transvaginal ultrasound is straightforward. Unlike later abdominal scans, you typically do not need a full bladder. In fact, a partially full or empty bladder is often more comfortable for a transvaginal scan. You may be asked to empty your bladder just before the procedure. Wear comfortable, loose-fitting clothing that’s easy to change out of, like a dress or pants with a stretchy waistband.
During the scan, you’ll lie on an exam table with your feet in stirrups. The sonographer will cover the transvaginal probe with a protective sheath and lubricant and gently insert it. You may feel some pressure, but it should not be painful. The room will be dimly lit, and you’ll see the images on a monitor. The sonographer will take measurements and may point out key structures. They are usually focused on the technical aspects and may not engage in extensive commentary, but don’t hesitate to ask questions like, "Can you point out the heartbeat?" or "Is that the yolk sac?" Many clinics allow you to record the heartbeat sound on your phone.
Practical Tips for a Smooth Experience
- Bring your partner or support person. This is a shared moment.
- Ask for a printout or video clip. Most places provide a black-and-white thermal print or a digital clip of the heartbeat. This is your first baby picture!
- Breathe and relax. Tensing up can make the scan more uncomfortable.
- Prepare questions in advance. Write down any concerns about pain, bleeding, or your medical history to discuss with your doctor after the scan.
- Understand the timing. If your dates are off, you might be earlier or later than 7 weeks, which could affect what’s visible. Be prepared for a possible follow-up.
Decoding the Results and Next Steps
After the 7 week sonography, the sonographer’s findings are sent to your obstetrician or midwife. You will have a follow-up appointment to discuss the results in detail. The doctor will interpret the measurements, confirm the dating, and explain what everything means for your pregnancy. If everything is normal and progressing well, your next routine ultrasound will likely be the nuchal translucency scan between 11-14 weeks, which combines early anatomy assessment with screening for certain chromosomal conditions.
If the scan shows any concerns—such as a borderline heartbeat, an irregular sac, or a suspected multiple pregnancy—your provider will outline the next steps. This might involve a repeat scan in one to two weeks to check for growth and development, blood tests (like a quantitative hCG and progesterone), or a referral to a maternal-fetal medicine specialist for high-risk care. The key is to remember that one snapshot in time is just that; trends over time are more important than a single measurement.
Building Your Prenatal Care Timeline
This first scan establishes your "gestational age" based on the embryo’s size, which is more accurate than dating by LMP alone. This new due date becomes the official timeline for all subsequent tests: the first-trimester screening, the anatomy scan at 20 weeks, and the glucose test. It synchronizes your entire prenatal care plan.
Conclusion: Embracing the First Milestone
The 7 week pregnancy sonography is far more than a routine medical procedure; it is the foundational cornerstone of your prenatal journey. It transforms hope and possibility into measurable, visual evidence of new life. From confirming a safe, intrauterine environment and detecting that miraculous first heartbeat to identifying multiples and establishing an accurate due date, the information gleaned from this early scan is indispensable for ensuring your health and your baby’s well-being.
While the images may be small and the details simple, the implications are profound. This scan provides the first layer of reassurance, guides all future medical decision-making, and offers parents that irreplaceable first connection. Approach your appointment with knowledge, prepare questions for your provider, and allow yourself to feel the wonder of seeing that tiny, flickering sign of life. It is the first of many remarkable glimpses you will have into your baby’s developing world, a moment that marks the true beginning of the tangible pregnancy experience. Trust the process, celebrate the heartbeat, and look forward to the incredible journey ahead, now firmly anchored by the evidence of this first, beautiful scan.