Lyme Disease In Dogs: That Bright Red Circle On Your Pet's Belly Explained
Have you ever noticed a strange, bright red circle on your dog’s belly and wondered, “What in the world is that?” It’s a sight that can stop any pet parent in their tracks. While there are many reasons for skin changes in our furry friends, one of the most concerning—and often misunderstood—connections is to Lyme disease. That circular rash, sometimes resembling a target or “bull’s-eye,” is a classic sign of a tick-borne illness, but it’s far more complex in dogs than in humans. This guide will dive deep into what that red circle means, how it relates to Lyme disease, and, most importantly, what you need to do to keep your canine companion safe and healthy.
The Mysterious Red Circle: Erythema Migrans in Dogs
When people think of Lyme disease, the first image that comes to mind is often the “bull’s-eye” rash, medically known as erythema migrans. It’s a hallmark symptom in humans, appearing at the site of the tick bite. But what about dogs? Do they get the same rash?
The answer is a nuanced yes, but with a critical caveat. Dogs can develop a skin lesion at the site of an infected tick attachment, but it’s significantly less common and often much harder to spot than in humans. This lesion may appear as a red, circular patch, sometimes with a darker center, mimicking the classic description. However, studies suggest that only a small percentage of infected dogs—estimates often range from 5-10%—ever show this visible skin sign.
Why is it so rare and elusive? Several factors come into play. A dog’s fur coat is the first and biggest obstacle. The rash typically forms directly where the tick was attached, which is often in hidden, hard-to-see areas: the belly, groin, armpits, base of the tail, or between the toes. By the time the rash becomes noticeable, the tick is long gone. Furthermore, the rash itself may be transient, fading quickly, or so subtle it’s mistaken for a minor irritation, insect bite, or allergy. Many pet owners never see it, which is why relying on this sign alone to diagnose or rule out Lyme disease is a dangerous mistake.
Understanding Lyme Disease: More Than Just a Rash
To grasp the significance of that red circle, we must first understand the disease it might signal. Lyme disease, or Lyme borreliosis, is a bacterial infection caused primarily by Borrelia burgdorferi and transmitted through the bite of infected black-legged ticks (Ixodes scapularis and Ixodes pacificus in North America).
The lifecycle of the tick is crucial. Nymphal ticks, which are tiny (about the size of a poppy seed), are the primary culprits for transmission because they are hard to detect and often go unnoticed. An infected tick must usually be attached for 36-48 hours or more to transmit enough bacteria to cause infection. This means regular tick checks are a powerful preventive tool.
Once transmitted, the bacteria travel through the bloodstream, potentially causing systemic inflammation. In dogs, the most common and serious manifestation is lameness due to Lyme arthritis. This is often sudden-onset, shifting-leg lameness—where the dog limps on one leg, then another—caused by inflammation in one or more joints. Other symptoms can include fever, lethargy, loss of appetite, and swollen lymph nodes. In some severe, untreated cases, the bacteria can damage the kidneys (Lyme nephritis), which is a life-threatening condition.
The key takeaway? The absence of a visible rash does NOT mean your dog is safe from Lyme disease. The majority of infected dogs will not show the skin lesion but may develop painful joint issues or other systemic signs.
What to Do If You Spot a Red Circle on Your Dog’s Belly
Discovering any unexplained skin change on your pet warrants attention, but a circular red patch should prompt specific action. Here is a step-by-step guide for concerned pet owners.
Step 1: Stay Calm and Conduct a Thorough Inspection
Do not panic. A red circle can have many causes, from a simple allergic reaction to a minor trauma. Immediately and gently part your dog’s fur in the area to get a clear look. Note the size, shape, color, and whether the center is different. Check for other signs: is there a scab? Is your dog scratching or licking it excessively? While you’re at it, perform a full-body tick check. Pay meticulous attention to the belly, groin, armpits, ears, neck, and between the toes. Use a flashlight if needed.
Step 2: Assess for Other Symptoms
Scan your dog for any additional signs of illness that have appeared recently. Ask yourself:
- Has my dog been limping or favoring a leg, even intermittently?
- Is he/she more tired than usual, reluctant to go for walks or play?
- Is there a loss of appetite or a low-grade fever (warm ears, dry nose)?
- Have there been any changes in drinking or urination habits?
Step 3: Contact Your Veterinarian Immediately
This is the most critical step. Do not wait to see if it gets better. Call your vet, describe what you see (“I’ve found a circular red patch on my dog’s belly, about the size of a quarter”), and schedule an appointment. Be prepared to answer questions about recent outdoor activities, tick prevention use, and any observed symptoms. Your vet’s guidance is essential.
Diagnosis: How Vets Confirm Lyme Disease
Diagnosing Lyme disease in dogs is a multi-step process that goes far beyond looking at the skin. Your veterinarian will employ a combination of history, physical exam, and diagnostic testing.
The Physical Examination
Your vet will conduct a comprehensive exam, checking joints for swelling or pain, palpating lymph nodes, and assessing overall demeanor. They will thoroughly examine the skin lesion and the entire coat for ticks or tick attachment sites.
Blood Tests: The SNAP 4Dx and Beyond
The most common initial screening is the SNAP 4Dx test (or similar combo tests). This in-clinic test checks for antibodies (the immune system’s response) to Borrelia burgdorferi (Lyme), as well as other common tick-borne diseases like Anaplasmosis, Ehrlichiosis, and Heartworm. A positive result indicates exposure to the Lyme bacteria, not necessarily active disease. Many dogs exposed will never get sick; their immune systems contain the infection.
For dogs with symptoms (like lameness or the red rash), a positive antibody test, combined with clinical signs, often confirms a diagnosis of active Lyme disease. In ambiguous cases, your vet may recommend a quantitative PCR test (polymerase chain reaction) on blood or joint fluid to look for the actual bacterial DNA, which is a stronger indicator of active infection. They may also run a urine protein:creatinine ratio test to screen for early kidney involvement, which is crucial for prognosis.
Treatment and Management: Getting Your Dog Back on Track
The good news is that Lyme disease is highly treatable in dogs with appropriate veterinary care. The standard treatment is a course of doxycycline, an antibiotic, typically administered for 28 days. For dogs that cannot tolerate doxycycline (e.g., young puppies, pregnant dogs), other antibiotics like amoxicillin may be used.
- Pain Management: For dogs with significant joint pain or lameness, your vet may also prescribe non-steroidal anti-inflammatory drugs (NSAIDs) like carprofen or meloxicam to reduce inflammation and provide comfort.
- Supportive Care: Rest is vital during treatment. Limit your dog’s activity to short leash walks for bathroom breaks to prevent further joint stress.
- Follow-Up Testing: After completing antibiotics, your vet will likely recommend a follow-up quantitative antibody test (like the Lyme Quantitative PCR or a repeat SNAP) to ensure antibody levels are declining, indicating the infection is being cleared. They will also recheck urine for protein.
For the rare cases where kidney disease (Lyme nephritis) has developed, treatment becomes more intensive, involving specialized diets, fluid therapy, and potentially other immunosuppressive drugs. Early detection and treatment are key to preventing these severe complications.
Prevention: Your First and Best Defense
Preventing Lyme disease is infinitely easier and less costly than treating it. A multi-layered approach is the gold standard.
1. Consistent, Vet-Recommended Tick Prevention
This is non-negotiable. Use a ** veterinarian-recommended tick preventive product** every single month, without fail, year-round. Ticks can be active in cooler weather. Options include:
- Topical treatments (e.g., fipronil, selamectin, permethrin—note: permethrin is for dogs only, never use on cats).
- Oral chewables (e.g., afoxolaner, fluralaner, sarolaner).
- Tick collars (e.g., seresto collar, effective for up to 8 months).
- Sprays and shampoos can be useful for immediate kill but are not long-term preventives.
Never use a product meant for cats on your dog, and vice-versa.
2. Daily Tick Checks and Safe Removal
After any outdoor adventure, especially in wooded or grassy areas, perform a thorough tick check. Use your fingers to feel through the fur, focusing on the head, neck, and ears. If you find a tick:
- Use fine-tipped tweezers or a tick removal tool.
- Grasp the tick as close to the skin’s surface as possible.
- Pull upward with steady, even pressure. Do not twist or jerk, as this can leave mouthparts behind.
- Clean the bite area and your hands with rubbing alcohol, iodine scrub, or soap and water.
- Do not use folklore methods like burning it with a match or covering it with petroleum jelly. These can cause the tick to regurgitate more bacteria into your dog.
3. Landscape Management
Make your yard less tick-friendly:
- Keep grass mowed short.
- Clear tall grasses, brush, and leaf litter.
- Create a barrier of wood chips or gravel between wooded areas and recreational zones.
- Consider using tick control treatments in your yard, focusing on shaded, humid edges.
4. Vaccination
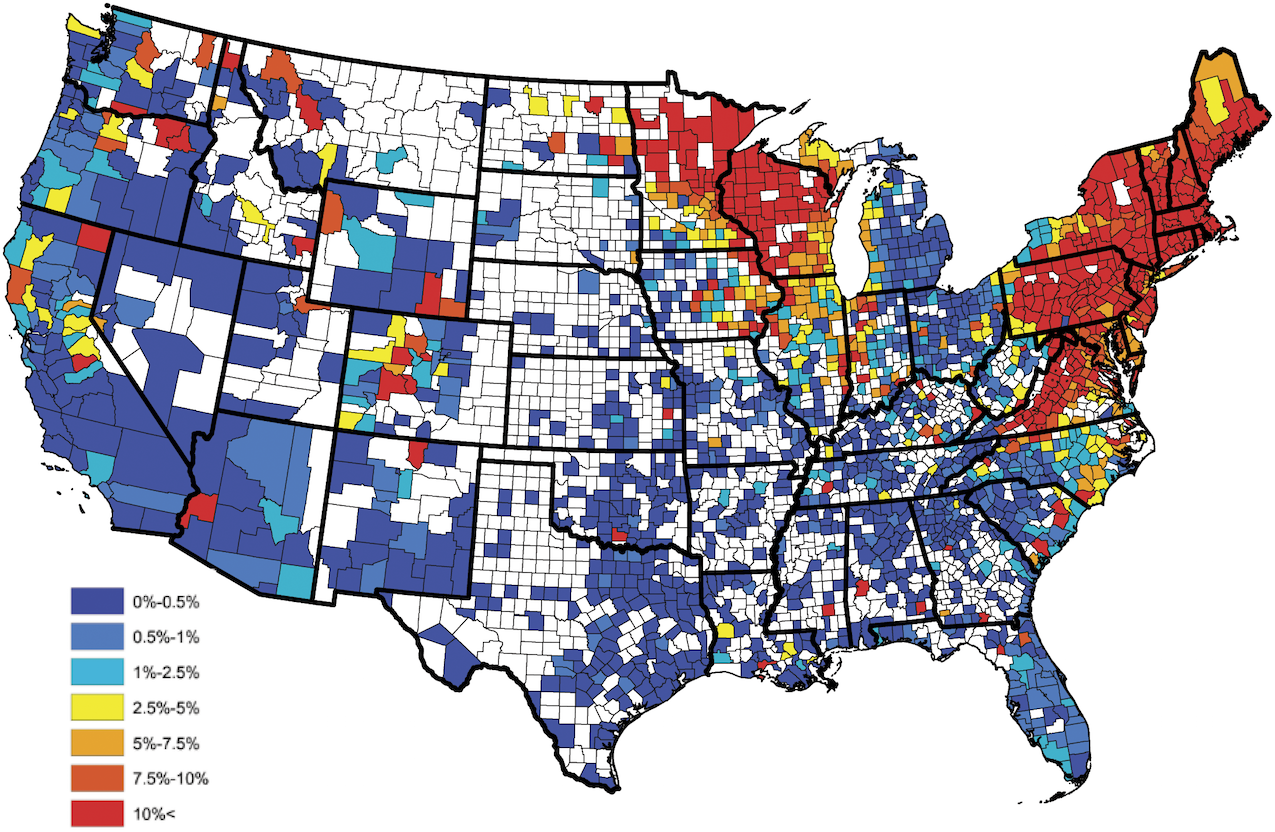
A Lyme disease vaccine is available for dogs. It is not considered a “core” vaccine and is recommended based on lifestyle and geographic risk (e.g., you live in or travel to a high-Lyme prevalence area like the Northeast, Mid-Atlantic, Upper Midwest, or parts of the West Coast). Discuss the pros and cons with your veterinarian. The vaccine does not provide 100% protection and is not a substitute for tick preventives.
Debunking Myths: What That Red Circle Is NOT
Misinformation about Lyme disease can cause unnecessary panic or, worse, dangerous delays in care. Let’s clarify a few points.
- Myth: The bull’s-eye rash is the main sign of Lyme in dogs.
- Fact: It’s rare and unreliable. Lameness is the #1 clinical sign.
- Myth: If I don’t see a tick, my dog can’t have Lyme.
- Fact: Nymphal ticks are poppy-seed sized and nearly invisible. The bite is often painless and unnoticed.
- Myth: A positive Lyme test means my dog is very sick.
- Fact: It means exposure. Many dogs are asymptomatic carriers. Treatment is based on symptoms, not just a positive test.
- Myth: Lyme disease is always fatal.
- Fact: With prompt antibiotic treatment, the prognosis for uncomplicated Lyme arthritis is excellent. The fatal form (kidney disease) is rare but serious.
- Myth: I can catch Lyme directly from my dog.
- Fact: Lyme is only transmitted through the bite of an infected tick. You cannot get it from your dog licking you, sharing saliva, or from its blood.
When to Worry: Red Flags That Need Immediate Vet Attention
While a red circle alone isn’t an emergency, certain combinations of symptoms require urgent veterinary care:
- The red circle is accompanied by sudden, severe lameness in one or more legs.
- Your dog is extremely lethargic, has a high fever, or is vomiting.
- There are signs of kidney trouble: increased thirst and urination, lethargy, nausea, or pale gums.
- You live in or have recently visited a high-risk Lyme area and find any unexplained skin lesion or your dog shows any illness.
- Your dog is not responding to standard treatment for another condition.
Remember, with tick-borne diseases, time is often joint health and kidney function. Err on the side of caution and get your dog checked.
Conclusion: Knowledge is Your Best Protection
That bright red circle on your dog’s belly is a potential clue, but it’s only one piece of a much larger puzzle. Lyme disease in dogs is a stealthy opponent, often operating without the dramatic “bull’s-eye” warning sign we see in humans. The real sentinels are the subtle changes in your dog’s gait, energy, and appetite.
Your role as a pet parent is clear: be vigilant, be preventive, and be proactive. Implement year-round tick control without exception. Perform those daily tick checks after adventures. Know the signs of Lyme arthritis—that shifting leg limp. And most importantly, partner with your veterinarian. Discuss your dog’s specific risk based on where you live and play. If you see anything unusual, like a mysterious red patch, make that call. Early detection and treatment are the keys to ensuring that a tick bite doesn’t turn into a long-term health struggle. By staying informed and consistent with prevention, you can help your dog enjoy many more years of happy, healthy, and itch-free adventures by your side.