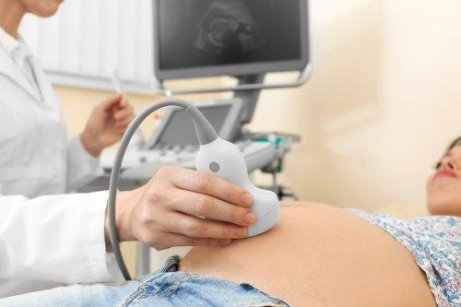
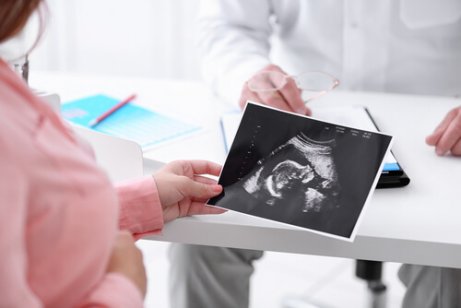
How Many Ultrasounds During Pregnancy? Your Complete Timeline Explained
How many ultrasounds during pregnancy will you actually have? It’s one of the first questions on every expectant parent’s mind, and for good reason. These magical windows into your baby’s world are more than just the “baby bump” photos you post on social media. They are critical diagnostic tools that monitor growth, detect potential issues, and provide unparalleled peace of mind. But navigating the pregnancy ultrasound schedule can feel confusing. Guidelines vary, and your personal journey might differ from your friend’s or sister’s. Is there a magic number? What does each scan check for? And are they truly safe for your developing baby? This comprehensive guide will demystify the entire ultrasound timeline during pregnancy, breaking down the standard protocol, the “why” behind each scan, and the factors that might change your personal count. By the end, you’ll know exactly what to expect and feel empowered to have informed conversations with your healthcare provider about your prenatal imaging plan.
The Standard Protocol: Typical Ultrasounds in a Low-Risk Pregnancy
For a healthy, low-risk pregnancy, major medical organizations like the American College of Obstetricians and Gynecologists (ACOG) outline a framework for ultrasound use during pregnancy. While it’s not a one-size-fits-all prescription, the consensus points to a series of key scans that provide essential information at crucial developmental stages. Think of it as a scheduled check-up plan for your baby, with each prenatal ultrasound serving a distinct purpose. The typical number falls between 2 to 3 diagnostic ultrasounds, but this can easily increase based on individual circumstances. Understanding this baseline is the first step to managing your expectations and recognizing when additional scans are medically necessary versus optional keepsakes.
The First Trimester Scan (Around 8-14 Weeks)
Often called the dating scan or viability scan, this is typically your first official ultrasound. Its primary job is to confirm the pregnancy is intrauterine (inside the uterus), check for a fetal heartbeat, and—most importantly—establish an accurate gestational age. By measuring the tiny embryo or fetus from crown to rump (the CRL measurement), your sonographer can predict your due date with remarkable precision, often within 3-5 days. This is far more accurate than dating by your last menstrual period, especially if your cycles are irregular. For many parents, this is the breathtaking moment they first see their baby, a speck of light with a flickering heartbeat. It also checks for multiple pregnancies (twins, triplets, etc.) and assesses basic early anatomy. If you’re considering non-invasive prenatal testing (NIPT) for chromosomal conditions, this scan may be used to confirm the gestational age needed for accurate test interpretation.
The Second Trimester Anatomy Scan (Around 18-22 Weeks)
This is the most detailed and comprehensive ultrasound of your pregnancy, often referred to as the mid-pregnancy scan or anomaly scan. It’s a head-to-toe, system-by-system examination of your baby’s development. The sonographer will meticulously measure the baby’s head, abdomen, and femur bone to ensure growth is on track. They will examine the brain’s structure (including the cerebellum and ventricles), the face (looking for cleft lip/palate), the spine, the heart’s four chambers and outflow tracts, the stomach, kidneys, bladder, and limbs. They will check the placenta’s location, maturity, and its relationship to the cervix (to rule out placenta previa), and measure the amniotic fluid index and cervical length. This scan is the primary screening tool for major structural birth defects. You’ll receive a detailed report, and if any soft markers or potential concerns are seen, your provider will discuss follow-up options, which may include a repeat scan or a more specialized level II ultrasound with a maternal-fetal medicine (MFM) specialist.
The Third Trimester Growth Scan (Around 28-32 Weeks, if indicated)
Not always routine for low-risk pregnancies, this growth ultrasound becomes more common in the final trimester. Its main goals are to assess the baby’s size (weight estimate), growth trajectory, amniotic fluid levels, placental position and function, and the baby’s position (head-down, breech, etc.). It’s particularly recommended if you have risk factors like hypertension, diabetes, a history of small babies, or if your fundal height measurements (the tape measure around your belly) aren’t matching your gestational age. This scan helps identify conditions like intrauterine growth restriction (IUGR) or polyhydramnios/oligohydramnios (too much or too little amniotic fluid). It provides a crucial snapshot of your baby’s well-being as they prepare for birth and can inform decisions about the timing and mode of delivery.
Why Your Ultrasound Count Might Differ: Personalized Factors
The “typical 2-3 scan” plan is a starting point, but your personal ultrasound schedule is a dynamic document, tailored by your health history and your baby’s development. Several factors can increase the number of diagnostic ultrasounds in pregnancy.
High-Risk Pregnancies Require Closer Monitoring
If you have pre-existing conditions like chronic hypertension, type 1 or type 2 diabetes, kidney disease, or autoimmune disorders, you’ll likely be under the care of a high-risk specialist (MFM). These conditions can affect placental function and fetal growth, necessitating more frequent monitoring. Serial ultrasounds—often every 3-4 weeks in the third trimester—become standard to track growth trends and amniotic fluid. Similarly, pregnancy-specific complications like gestational diabetes (especially if poorly controlled), preeclampsia, or a history of preterm labor or stillbirth will prompt a more vigilant ultrasound schedule.
Multiple Pregnancies: Twins, Triplets, and Beyond
Carrying multiples automatically categorizes your pregnancy as high-risk. Twin pregnancy ultrasound schedules are inherently more intensive. You’ll have an early scan to confirm zygosity (identical or fraternal) and chorionicity/amnionicity (how many placentas and amniotic sacs), which is critical for managing risk. Then, you’ll typically have anatomy scans for each baby (often done in the same session) and regular growth scans every 3-4 weeks starting in the second trimester to ensure both babies are growing appropriately and to monitor for twin-to-twin transfusion syndrome (TTTS) in identical twins sharing a placenta.
Concerns Arising from Previous Scans or Screenings
Sometimes, the need for more ultrasounds arises directly from the findings of an earlier one. If the anatomy scan shows a “soft marker” (an ultrasound finding that slightly increases the chance of a chromosomal condition but isn’t diagnostic), your provider will recommend a follow-up scan by a specialist in a few weeks to see if it persists or resolves. A low amniotic fluid reading or a borderline placenta previa on an earlier scan will also trigger closer surveillance with repeat imaging.
The Safety and Science: Are Ultrasounds Harmless?
A fundamental concern for every parent is ultrasound safety during pregnancy. It’s natural to worry about exposing your developing baby to any technology. The overwhelming consensus from decades of research and organizations like the FDA and ACOG is that diagnostic ultrasound is safe when used appropriately. Unlike X-rays, it uses high-frequency sound waves, not ionizing radiation. There is no known evidence that it harms the fetus when performed by a qualified professional for medically indicated reasons.
However, the principle of “as low as reasonably achievable” (ALARA) is strictly followed. This means sonographers use the minimum necessary time and power settings to obtain the required diagnostic information. The key distinction is between medically necessary diagnostic ultrasounds and non-medical “keepsake” or “entertainment” ultrasounds. The latter, often done in mall boutiques without a medical indication, are not endorsed by medical societies. They can involve longer scan times and settings optimized for 3D/4D images rather than diagnostic quality, potentially exposing the baby to unnecessary energy. Always ensure your ultrasounds are prescribed by your doctor or midwife and performed in a certified medical setting by a registered diagnostic medical sonographer (RDMS) with experience in obstetrics.
Practical Preparation: Making the Most of Your Ultrasound Appointments
Knowing how to prepare for a pregnancy ultrasound can reduce anxiety and improve the experience. For early scans, a full bladder is often required as it acts as a “window” to better see the uterus. You’ll be asked to drink 24-32 ounces of water an hour before and not urinate. For later scans, a full bladder is less critical, but a comfortably full bladder can still help. Wear comfortable, loose-fitting clothing that’s easy to part or lift. Have your questions written down beforehand. The sonographer is not allowed to diagnose or give you news; their role is to acquire images for the interpreting physician. Bring your partner or a support person if you’d like. Understand that the anatomy scan is a detailed screening test, not a guarantee. Its purpose is to detect major anomalies; some conditions cannot be seen on ultrasound. Finally, be prepared for the possibility of an “incomplete” scan if the baby is in an unfavorable position. This is common and usually just means you’ll be asked to walk around or reschedule for another day.
Addressing Common Questions and Myths
Q: Can too many ultrasounds harm my baby?
A: As stated, when performed for valid medical reasons by trained professionals, there is no evidence of harm. The risk is considered negligible compared to the benefit of obtaining crucial diagnostic information. The concern is with unnecessary scans without a medical indication.
Q: What about the 3D/4D “bonding” scans?
A: These are optional and not part of standard medical care. They can be a wonderful way to see your baby’s face, but they should be done in addition to, not instead of, your medically necessary diagnostic scans. Choose a reputable facility that prioritizes safety.
Q: My insurance only covers 2 ultrasounds. What do I do?
A: This is a common frustration. First, understand why your provider is recommending a scan. If it’s medically necessary (e.g., checking growth due to diabetes), your provider can often submit a letter of medical necessity to get it covered. If it’s a “routine” third-trimester scan for a low-risk pregnancy, your provider may decide it’s not essential and skip it. Have an open conversation with your provider about the medical rationale and cost implications.
Q: What if an abnormality is found?
A: This is a parent’s worst fear. Remember, the anatomy scan is a screen. If a potential issue is identified, the next step is usually a targeted follow-up ultrasound with a specialist (MFM) and possibly other tests like amniocentesis or cell-free DNA testing for more definitive answers. Not all findings lead to a diagnosis, and many “soft markers” are benign. Your care team will guide you through the steps.
The Emotional Journey: Ultrasounds as More Than Medical Tools
Beyond the clinical data, pregnancy ultrasounds are profound emotional milestones. They transform an abstract idea of a baby into a tangible, moving reality. Seeing that first flutter of a heartbeat, the yawn, the thumb-sucking, the kick—these moments create an irreplaceable bond. It’s okay to look forward to these appointments as much for the joy as for the information. Bring your partner, record the heartbeat on your phone (if allowed), and savor the view. However, it’s also important to manage expectations. The images are not always the clear, glossy photos you see online. Baby’s position, your body habitus, and amniotic fluid levels can affect image quality. The sonographer’s primary job is to check measurements, not produce portrait-quality photos. Be kind to them and appreciate their expertise in gathering the medical data your doctor needs.
Conclusion: Your Ultrasound Plan, Your Pregnancy
So, how many ultrasounds during pregnancy will you have? The definitive answer is: it depends. The standard blueprint of a dating scan, an anatomy scan, and possibly a growth scan provides a solid foundation for a low-risk pregnancy. Yet, your unique health profile, your baby’s development, and any arising concerns will dictate the final count. The most important takeaway is to view ultrasounds not as a tally to be met, but as essential, personalized tools in your prenatal care toolkit. They are scheduled at key moments to answer critical questions about your baby’s growth, anatomy, and well-being. Trust the guidance of your obstetrician or midwife. Ask them directly: “Based on my history, what is your recommended ultrasound schedule for me, and why?” Understanding the medical purpose behind each scan empowers you to be an active participant in your care. Embrace the diagnostic power of these scans for the vital information they provide, and cherish the precious glimpses they offer into the incredible life growing within you. Your pregnancy journey is unique, and so is your ultrasound timeline—crafted to ensure the healthiest outcome for both you and your baby.